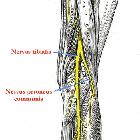
piriformis syndrome



Piriformis syndrome is a rare entrapment neuropathy resulting in radicular pain radiating into the buttock and hamstrings. The entity is controversial as are the putative causes.
Clinical presentation
Sciatic pain reproduced on passive internal rotation/adduction of a flexed hip is considered suggestive of the syndrome.
Pathology
The general, although by no means unanimous, consensus is that piriformis syndrome is caused when hypertrophy, inflammation, injury or anatomical variation of the piriformis muscle results in compression of the sciatic nerve as they both exit the pelvis through the greater sciatic notch.
Normally, the sciatic nerve typically passes immediately anterior to the piriformis muscle. This relationship is variable, however, as the nerve occasionally passes through the muscle, or splits early, with part of it passing through the muscle.
Additionally, an accessory piriformis muscle that arises from the more medial part of the sacrum can be implicated.
Etiology
- early sciatic nerve division and passage through the muscle belly or above it
- narrowed sciatic foramen
- accessory piriformis muscle
- muscle hypertrophy
- lumbar lordosis
- ganglion or cyst
- any mass lesion
- spasm
- athletes
- cerebral palsy
- bursitis and inflammation
Radiographic features
MRI
MRI is the only modality which can adequately visualize the region. The radiographic appearance depends on the cause, and often no abnormality is noted. If muscle injury or inflammation are present then increased signal within the piriformis muscle may be seen on T2 MRI. An accessory piriformis muscle may be identified.
Treatment
- physiotherapy with stretching (especially if spasm is thought to be the cause)
- administration of non-steroidal anti-inflammatory agents
- injection of local anesthetic and steroid
- injection of botulinum toxin to atrophy the piriformis muscle
- surgical release of the piriformis muscle
- neurolysis
History and etymology
Entrapment of the sciatic nerve by the piriformis muscle was first described By W Yeoman in 1928 .
Differential diagnosis
Clinically it should be distinguished from hamstring syndrome.
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Piriformis-Syndrom:
Assoziationen und Differentialdiagnosen zu Piriformis-Syndrom: