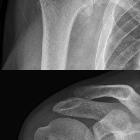
tibial plateau fracture

Tibial plateau fractures were originally termed a bumper or fender fracture but only 25% of tibial plateau fractures result from impact with automobile bumpers.
Pathology
The most common mechanism of injury involves axial loading, e.g. fall from a significant height. In younger patients, the most common pattern of fracture is splitting, while older, more osteoporotic patients, depression fractures typically are sustained.
Soft tissue injuries (e.g. to cruciate and collateral ligaments) occur in approximately 10% of patients.
Fractures of the lateral plateau are much more common than the medial plateau. To injure the medial plateau, a large amount of force is required; fractures of the medial plateau are usually seen in conjunction with fractures of the lateral plateau and other bones around the knee joint.
Radiographic features
Tibial plateau fractures are complex injuries that require adequate imaging to assess prior to fixation.
Plain radiograph
Plain radiography often underestimates the severity of the injury. Lipohemarthrosis should be present.
CT
CT is very helpful in accurately defining the extent of the bony injury and facilitates orthopedic intervention. The Schatzker classification is used in tibial plateau fractures.
MRI
MRI is very helpful in the assessment of soft tissue injury around the joint.
Treatment and prognosis
The goal of therapy is to reduce the fracture and begin early mobilization. If the patient is immobilized for a lengthy period (>3 weeks), the joint will not return to full range of movement.
Depression of a tibial plateau that is inadequately corrected results in a varus or valgus deformity and accelerated osteoarthritis.
Unappreciated ligamentous injury causes greater than normal stress on the remaining support structures of the joint, malalignment, and the development of premature osteoarthritis.
Siehe auch:
- Arthrose
- Frakturen der Eminentia intercondylaris tibiae
- Tibiafraktur
- Tibiakopffraktur AO-Klassifikation
- Schatzker-Klassifikation
- Trampolinfraktur
und weiter:

 Assoziationen und Differentialdiagnosen zu Tibiaplateaufraktur:
Assoziationen und Differentialdiagnosen zu Tibiaplateaufraktur: