tibial tuberosity avulsion fracture









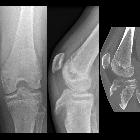
Tibial tuberosity avulsion fractures are uncommon.
Epidemiology
These fractures have an incidence 0.4% to 2.7%, and males are affected more-so than females. The typical patient is an adolescent male approaching skeletal maturity with well-developed quadriceps.
Associations
- patella tendon or quadriceps tendon rupture
- compartment syndrome due to the recurrent branch of the anterior tibial artery injury
- concomitant Osgood-Schlatter disease is common
Pathology
Typically caused by injuries from sporting activities involving jumping, most commonly basketball. Potential mechanisms:
- violent knee flexion against a tight contraction quadriceps, e.g. landing from a jump
- violent quadriceps contraction against a fixed foot, e.g. jumping
Classification
There are multiple classification systems with multiple modifiers. The most commonly used is the modified Ogden classification.
Modified Ogden classification (modification of Watson-Jones classification):
- type I: fracture of the secondary ossification center near the patella tendon insertion
- type II: fracture between the primary and secondary ossification centers
- type III: fracture that traverses the primary and secondary ossification centers (most common type)
- type IV: fracture through the entire physis
- type V: avulsion of the periosteal sleeve
- modifiers: A - nondisplaced and B - displaced
Watson-Jones classification:
- type 1: avulsion of the apophysis without injury to the tibial epiphysis
- type 2: epiphysis is lifted cephalad and incompletely fractured
- type 3: displacement of the proximal base of the epiphysis with the fracture line extending into the joint
Radiographic features
Plain radiograph
Recommended views include an AP and lateral knee radiograph. Optional views include an internal rotation view bringing the tibial tuberosity into profile or a contralateral knee radiograph for comparison.
Plain radiographs may demonstrate:
- widening of open apophysis typically demonstrating a displacement of proximal apophysis
- hemarthrosis if there is intra-articular extension
- patella alta
CT
CT is helpful to determine intra-articular or posterior extension.
Treatment and prognosis
All patients require a variable period of immobilization averaging 4 weeks.
- type I: usually non-operative immobilization in a long leg cast 4-6 weeks
- type II-V: usually surgical - closed reduction via percutaneous clamping and lag screw fixation or open reduction
Full range of motion is expected by 3 months, with a return to pre-injury level of activity thereafter.
See also
Siehe auch:
- Morbus Osgood-Schlatter
- Tubercule de Tillaux Chaput
- Avulsionsfraktur
- Klassifikation Apophysenfraktur der Tibia nach Watson-Jones
und weiter:

 Assoziationen und Differentialdiagnosen zu Avulsionsfraktur der Tuberositas tibiae:
Assoziationen und Differentialdiagnosen zu Avulsionsfraktur der Tuberositas tibiae:


