Aging blood on MRI





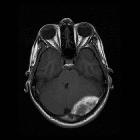



Hemorrhage on MRI has highly variable imaging characteristics that depend on both the age of the blood, the type of hemoglobin present (oxy- deoxy- or met-), on whether or not the red blood cell walls are intact and the specifics of the MRI sequence. Although MRI is often thought of as not being sensitive to acute hemorrhage, this is not, in fact, true particularly with more modern sequences .
The appearance of hemorrhage will, however, be different at different times and is not perfectly stereotyped, as such caution should be exercised in precisely aging hemorrhages.
Physiology
The factors that affect the appearance of hemorrhage on MRI vary according to the sequence. The oxygenation state of hemoglobin and the location of either contained within red blood cells or diffused in the extracellular space have a tremendous effect on the imaging effects of blood. The three hemoglobin states to be considered are oxyhemoglobin, deoxyhemoglobin and methemoglobin.
Oxyhemoglobin, accounting for 95% of hemoglobin in arterial blood and 70% in venous blood, is only weakly diamagnetic, having little T2* and only mildly shortening T1 relaxation time . This is the result of heme iron is in ferrous form (Fe2+) and has no unpaired electrons .
Deoxyhemoglobin, in contrast, having lost oxygen has four unpaired electrons and is strongly paramagnetic and results in substantial signal loss on T2* weighted sequences, such as susceptibility weighted imaging, and blooming artefact .
Methemoglobin results from oxidative denaturation of the heme molecule to the ferric (Fe3+) form has five unpaired electrons is also strongly paramagnetic .
T1 weighted sequences
Oxyhemoglobin and deoxyhemoglobin produce little effect on T1 signal. The presence of blood proteins results in intermediate T1 signal in hyperacute and acute hemorrhages.
T2* weighted sequences
T2* weighted sequences, such as susceptibility weighted imaging and gradient echo are primarily affected by the hemoglobin oxygenation state and whether or not cell lysis has occurred .
While contained within red blood cells, resulting in uneven distribution of paramagnetic effects, both deoxyhemoglobin and methemoglobin result in signal loss. Once the cells lyse and methemoglobin is distributed evenly throughout the clot, the local magnetic field distortion is also lost and T2 signal loss fades .
Eventually, hemosiderin and ferritin (both paramagnetic) are then ingested by monocytes and macrophages and results once more in unevenly distributed paramagnetic effects and signal loss .
Diffusion-weighted imaging
Apparent diffusion coefficient (ADC) maps demonstrate fairly stable values substantially lower than normal white matter in all stages except for chronic (see below), whereas isotropic/trace DWI images, due to them combining T2 and diffusion effects, demonstrated high signal only on hyperacute and late subacute phases .
Stages
In general, five stages of hematoma evolution are recognized:
- intracellular oxyhemoglobin
- isointense on T1
- isointense to hyperintense on T2
- high signal on isotropic DWI and reduced ADC values
- intracellular deoxyhemoglobin
- T2 signal intensity drops (T2 shortening)
- T1 remains intermediate-to-low
- low signal on isotropic DWI and reduced ADC values
- intracellular methemoglobin
- T1 signal gradually increases (T1 shortening) to become hyperintense
- low signal on isotropic DWI and reduced ADC values
- extracellular methemoglobin: over the next few weeks, as cells break down, extracellular methemoglobin leads to an increase in T2 signal
- high signal on isotropic DWI and reduced ADC values
- periphery
- intracellular hemosiderin
- low on both T1 and T2
- center
- extracellular haemichromes
- isointense on T1, hyperintense on T2
- low signal on isotropic DWI and increased ADC values
Remembering these may be facilitated by this aging blood on MRI mnemonic.
Practical points
- extracranial blood products age differently from intracranial blood products, and extracranial hematomas often have a heterogeneous appearance, confounding attempts at reliably dating the age of an extracranial hemorrhage
- subacute and chronic blood appears hypointense and blooms on MRI T2* weighted sequences (e.g. susceptibility weighted imaging (SWI))
- presence of blood products in a cavity will result in low ADC values and therefore make use of diffusion restriction to diagnose pus in an abscess useless
Siehe auch:

 Assoziationen und Differentialdiagnosen zu Altersbestimmung Blutung MRT:
Assoziationen und Differentialdiagnosen zu Altersbestimmung Blutung MRT:

