burst fracture









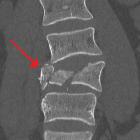







Burst fractures are a type of compression fracture related to high-energy axial loading spinal trauma that results in disruption of the posterior vertebral body cortex with retropulsion into the spinal canal.
Clinical presentation
They usually present as back pain and or lower limbs neurologic deficits in the clinical scenario of trauma.
Pathology
Burst fractures most commonly occur at L1 with the majority (~90%) occurring from T9-L5. Two-level burst fractures are much less common than single-level burst fractures .
Mechanism
It is a result of a high-energy compressive injury (axial loading), much like the Jefferson fracture. The intervertebral disc is driven into the vertebral body below.
Typically they occur following a fall from height (often landing on feet) or from a motor vehicle accident .
Radiographic features
General features include :
- loss of vertebral height on lateral views: anterior portion is commonly compressed more than the posterior portion of the vertebral body
- fracture always involves the posterior vertebral body cortex
- burst vertebral body on axial CT
- vertical fracture through the posterior elements is usually present in more severe trauma
- interpedicular widening
- bone fragment retropulsion into the spinal canal may occur
- consequent spinal cord contusion may occur, and it is best assessed by MRI (axial and sagittal T2)
Radiology report
- all patients require a CT to assess the injury and evaluate the extent of the retropulsed fragments which may enter the spinal canal, and a percentage of spinal canal narrowing should be reported
- caution must be taken when referring stability on the report, as this should be assessed together with the clinical data
Differential diagnosis
- other types of compression fracture: posterior vertebral body cortex is intact
- Chance fracture
- butterfly vertebra: well corticated congenital division of vertebrae seen on coronal images; no antecedent trauma history
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Berstungsfraktur:
Assoziationen und Differentialdiagnosen zu Berstungsfraktur:

