OPLL





















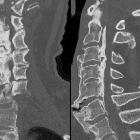



Ossification of the posterior longitudinal ligament (OPLL) is typically an entity seen in patients of Asian descent, although it is seen in all ethnic groups. It is characterized by, as the name suggests, ossification of the posterior longitudinal ligament.
Epidemiology
There is a recognized greater prevalence in males and in the elderly . There is also considerable racial variation:
- incidence in the Japanese/Asian population: 2.4%
- incidence in Caucasians: 0.2-0.7%
OPLL is twice as common in men compared with women.
Clinical presentation
Patients may be asymptomatic, or have evidence of radiculopathy and/or myelopathy . If present, symptoms usually manifest in the 4-6 decades of life .
Pathology
The exact pathogenesis of OPLL is rather unclear .
Associations
OPLL is often associated with several other entities:
- diffuse idiopathic skeletal hyperostosis (DISH)
- ossification of the ligamentum flavum
- ankylosing spondylitis
- schizophrenia: possible (in one study)
DISH may be seen in up to 12% of elderly male Caucasians, with OPLL seen in about half of these, suggesting the incidence among Caucasians may be higher than the figures above.
Location
This typically seen in the mid cervical spine and results in central canal stenosis, predisposing the patient to cord injury from minor trauma:
- cervical: 75%
- thoracic: 15%
- lumbar: 10%
Stages of spinal cord damage by OPLL
- stage 0: normal or mild compression of the anterior horn without neuronal loss
- stage 1: mild compression of the anterior horn with partial neuronal loss
- stage 2: marked deformity of anterior horn; severe neuronal loss
- stage 3: severe spinal cord damage
T2-weighted sequences are considered the most effective in the evaluation of spinal cord compression due to both the ossification and abnormal signal intensity of the spinal cord .
Types of OPLL
- type 1: continuous (ossification of several vertebral segments)
- type 2: segmental (several segments are affected, ossification is disrupted)
- type 3: mixed (mix of types 1 and 2)
- type 4: localized (circumscribed, only one or two segments)
Treatment and prognosis
Management can range from conservative to surgical removal. Surgical options can include an anterior, posterior or combined approach. An anterior approach (e.g. plated multilevel anterior discectomy and fusion, anterior cervical corpectomy with fusion) may provide more direct decompression and best improve myelopathy, although may cause greater soft-tissue morbidity. Posterior approaches (e.g. laminectomy and fusion and laminoplasty) may be better tolerated in older patients.
Siehe auch:
- Morbus Bechterew
- Fluorose
- Diffuse idiopathische Skeletthyperostose
- Ossifikation der Ligamenta flava
- verkalkte Bänder
- Ligamentum longitudinale posterius
- Verkalkung Ligamentum longitudinale anterius
- Chalk-Stick-Fraktur der HWS
und weiter:

 Assoziationen und Differentialdiagnosen zu Ossifikation Ligamentum longitudinale posterius:
Assoziationen und Differentialdiagnosen zu Ossifikation Ligamentum longitudinale posterius:





