Radiation-induced enteritis



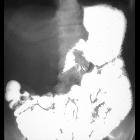
Radiation-induced enteritis is a small bowel pathology resulting from toxic effects of radiotherapy on the small bowel wall and vasculature.
Epidemiology
5-15% of patients treated with radiotherapy (usually >4500 cGy) develop chronic radiation enteropathy.
Terminology
Enteritis is inflammation of the small bowel. If there is concurrent inflammation of the large bowel, then enterocolitis is a better term.
Clinical presentation
The clinical presentation is non-specific with abdominal pain, vomiting, bloody diarrhea and steatorrhea. Patients with chronic radiation enteritis may develop deficiencies of calcium, iron and vitamin B12 deficiency.
Pathology
In the acute phase, radiation affects bowel mucosa causing cell death with ulceration. It also causes inflammation with mucosal and submucosal edema. In the subacute and chronic phases healing and fibrosis occurs. Additionally, radiation induces endarteritis obliterans, which results in a state of chronic mesenteric ischemia leading to bowel strictures.
Risk factors
- adhesions from previous abdominal surgery
- peritonitis prior to radiation therapy
- high radiation dose
- risk factors for atherosclerosis; hypertension and diabetes mellitus
- chemotherapy
Classification
- acute stage: concurrent or within 2 months of treatment
- subacute: 2-12 months after treatment
- chronic: >12 months after treatment
Radiographic features
Fluoroscopic enteroclysis
- acute radiation enteritis
- bowel loops appear spastic with luminal narrowing and edema of mucosal folds
- chronic radiation enteritis
- thickening of bowel wall and folds due to edema or fibrosis
- “stack of coins appearance” enlarged smooth, parallel mucosal folds
- single or multiple bowel stenoses
- ulcers
CT and MRI
- bowel wall thickening and luminal narrowing
- small bowel obstruction
- fistulas between the bowel (especially colon) and the bladder or vagina
Following pelvic radiotherapy, enteritis of the small bowel typically involves the more fixed terminal ileum and manifests as bowel wall thickening and submucosal edema at CT.
Differential diagnosis
General imaging differential considerations include:
- Crohn disease
- enteric metastases
- enteric lymphoma
- mesenteric ischemia
As a broader differential consider other forms of enteritis.
Siehe auch:

