sialography
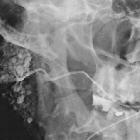








Sialography is the imaging of the salivary glands, most commonly the parotid gland. The salivary ducts are conventionally examined fluoroscopically with high sensitivity, though cross-sectional imaging with CT or MR sialography has also been described.
Indications
- suspected sialolithiasis or salivary duct obstruction
- suspected sialadenitis: to identify ductal strictures
- suspected sialectasis in chronic inflammatory disorders and autoimmune diseases
Types of sialography
There are three types:
- conventional/fluoroscopic sialography (with or without digital subtraction)
- CT sialography (ultrafast technique)
- MR sialography
In most cases, ultrasound (with sialography, if required) is an appropriate imaging modality for the investigation of ductal pathology. In cases of sialolithiasis, ultrasound of the parotid glands is a useful, readily available, noninvasive, and inexpensive option.
Procedure
Technique of conventional sialography
- control images are taken with the patient supine to assess for radiopaque calculi
- lateral oblique and anteroposterior views
- using tongue depressors for submandibular
- the patient may be asked to suck on a lemon or secretory stimulant for 2-3 minutes before sialography
- to make the salivary duct opening conspicuous for cannulation
- symptomatic parotid or submandibular duct cannulated
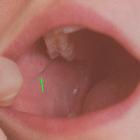
- 21 gauge catheter for Stensen's duct
- located adjacent to the crown of the second upper molar in the buccal mucosa
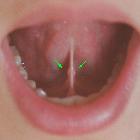
- 24 or 27 gauge for Wharton's duct
- at the base of the frenulum of the tongue
- 21 gauge catheter for Stensen's duct
- up to 2 mL of water-soluble contrast is instilled
- care should be taken not to introduce air into the salivary ducts, as it can mimic a ductal calculus on sialography
Advantages
- higher spatial resolution for superior diagnostic elucidation (when the procedure is successfully achieved) with accurate delineation of second- and third-order branches
- enables therapeutic approach in sialoendoscopy for removal of sialoliths, retrograde displacement of sialoliths to relieve acute obstruction, and to dilate strictures
Disadvantages
- invasive procedure
- the substantial failure rate of the procedure (especially submandibular sialography) is due to cannulation problems, lack of skill, lack of patient compliance, pain, etc.
- radiation exposure
- contrast media exposure with risk of allergic reaction
Technique of CT sialography
The procedure is essentially the same as a conventional sialogram, after which the patient is positioned in a CT in a neutral supine position. Multiplanar data acquisition allows for 3D reconstruction. Intravenous contrast material can be administered for better soft tissue evaluation, especially for parotid masses. In the 1970s and 1980s, when this technique was first introduced, slower CT scans called for delayed ductal emptying, for which atropine was given.
Advantages
- assessment of glands other than the parotids is possible
- better diagnosis of parenchymal pathology, excellent visualization of the deep lobe, and better subtraction options
- no special positioning required
Disadvantages
- intravenous atropine is required to minimize run-off of contrast and impair ductal clearance in some cases
- radiation exposure
- invasive procedure
Technique of MR sialography
MRI sialography is a fairly sensitive and reliable method of evaluating the salivary glands. Fast acquisition heavily T2 weighted sequences (e.g. RARE, CISS, FISP, as used in MRCP and MR urography) brighten intraluminal fluid and display ductal morphology adequately with no need to inject contrast into the ducts. MR contrast administered intravenously is a useful adjunct.
Advantages
- rapid acquisition
- non-invasive
- assessment of other glands possible
- excellent delineation of parenchymal pathology
- no special positioning required
- because no cannulation is required, the risk of air bubbles simulating intraductal calculi is minimized
Disadvantages
- general MRI contraindications, e.g. pacemakers, implants, claustrophobia
- dental fillings, implants, bridges, etc. can cause image impairment
- only first- and second-order branches can be delineated
See also
Siehe auch:
- Sjögren-Syndrom
- Caruncula sublingualis
- Speichelstein Ductus submandibularis
- Papilla parotidea
- CT-Sialographie
- Fistel in der Sialographie
- kindliche Sialektasie
- MRT-Sialographie
- Trauma der Speicheldrüsen
und weiter:

 Assoziationen und Differentialdiagnosen zu Sialographie:
Assoziationen und Differentialdiagnosen zu Sialographie:

