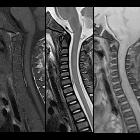
spinal epidural hematoma


Spinal epidural hematomas (EDH) are a rare spinal pathology which can result in serious morbidity with delayed or non-treatment. They are typically considered a surgical emergency.
Clinical presentation
The patient's symptoms and signs will depend on the location of the EDH, and degree of spinal cord / cauda equina compression, but invariably there will be a combination of severe pain and neurological deficit. See spinal cord injury and cauda equina syndrome for more information.
Pathology
Spinal EDH is most commonly spontaneous venous bleeds, often in the setting of coagulopathy or over-anticoagulation. They are anatomically located in what is known as the extradural neural axis compartment, located between the dura propria (visceral layer) and periosteum.
Etiology
- spontaneous (most common )
- especially in the context of a bleeding disorder or over-anticoagulation
- trauma, e.g. vertebral fracture
- iatrogenic, e.g. lumbar puncture, epidural anesthesia
- spinal arteriovenous malformations or other vascular anomalies
- spinal tumors
- pregnancy
Location
Spinal EDH can occur throughout the spine but is most common in the cervicothoracic region, usually posterior to the thecal sac over 2-4 vertebral levels .
Radiographic features
CT
- non-contrast: hyperdense (50-70 HU) extradural mass
MRI
Signal characteristics will vary on the age of the blood. Signal characteristics of acute spinal EDH :
- T1: isointense or hyperintense to spinal cord
- T2: heterogeneously hyperintense to spinal cord with hypointense foci
- T2*: blooming artifact
Differential diagnosis
Practical points
- assessment of spinal cord compression and spinal nerve roots should always be done
Siehe auch:
- epidurale intraspinale Raumforderung
- extramedulläre Hämatopoese
- epidurales Hämatom
- extraossäres Plasmozytom
- spinales subdurales Hämatom
- spinaler Epiduralabszess
- intraspinale Blutungen
und weiter:

 Assoziationen und Differentialdiagnosen zu spinales epidurales Hämatom:
Assoziationen und Differentialdiagnosen zu spinales epidurales Hämatom: