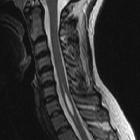
Tethered cord syndrome



















Tethered cord syndrome is a neurological disorder caused by tissue attachments that limit the movement of the spinal cord within the spinal canal.
Clinical presentation
Tethered cord syndrome is a clinical diagnosis based on neurologic deterioration involving the lower spinal cord . Patients may present with any combination of the following :
- progressive leg weakness or sensory loss
- disturbance of bowel or bladder function
- low back pain or sciatica
- spinal deformities such as scoliosis
- foot deformities such as pes cavus
- cutaneous stigmata of spinal dysraphism (e.g. hairy patch, dimple, subcutaneous lipoma)
The condition typically presents in children but occasionally goes undiagnosed until or is acquired in adulthood.
Pathology
As the spinal column grows faster than the cord, tethering lesions cause progressive stretching of the spinal cord. Abnormal traction leads to chronic ischemic changes and neuronal dysfunction.
Etiology
Tethered cord syndrome is associated with most of the major types of spinal dysraphism, except isolated bifid vertebrae (spina bifida occulta) and neurenteric cysts . Moreover, as open spinal dysraphism (mostly myelomeningocele) must be repaired in the neonatal period, those patients with this history who develop tethered cord syndrome do so years later due to adhesions rather than the dysraphism itself .
Thus, the most common causes of tethered cord syndrome are the closed spinal dysraphisms in the spectrum of spinal lipomas (lipomyelomeningocele, conus lipoma, and filar lipoma) and the tight filum terminale (with or without filar lipoma) . Other causes include arachnoid adhesions (due to trauma/surgery or infection/inflammation), split cord malformation (diastematomyelia and diplomyelia), dermal sinus tracts, and dermoid/epidermoid tumors .
Classification
Classifications of etiologies as "primary" or "secondary" tethered cord syndrome are heterogeneous and conflicting in the literature. For instance, primary tethered cord syndrome may refer to all congenital causes in general, closed spinal dysraphisms as a group, or tight filum terminale in particular . Without a consensus nomenclature, these terms are best avoided.
Radiographic features
Most commonly, the conus medullaris terminates in a low position below the level of the L2 vertebral body . However, tethered cord syndrome is possible in the setting of a normal conus position .
Additional imaging features depend on the etiology, which are described separately:
- spinal lipomas
- lipomyelomeningocele
- conus lipoma
- filar lipoma
- tight filum terminale
- split cord malformation
- dorsal sinus
- dermoid cyst
Ultrasound
Ultrasound may be a useful screening exam and may be of use in the pediatric population. The lack of ossification of the posterior arch of the spine in normal infants and the presence of a bony defect in patients with spina bifida permit sonographic examination.
MRI
MRI is useful in visualizing the conus medullaris, assessing the thickness of the filum terminale, identifying traction lesions, and evaluating associated bony dysraphisms.
Prone imaging may be useful in patients who have undergone tethered cord surgery or in those in whom clinical suspicion is high while supine MRI imaging demonstrated no abnormalities . Prone MRI imaging is however of little value when supine MRI has demonstrated a causative abnormality.
Treatment and prognosis
Untreated, tethered cord syndrome has a progressive course. Surgical release, in selected patients, can stabilize or improve function .
History and etymology
Tethered cord syndrome was coined in 1976 by the Canadian neurosurgeon Harold J Hoffman and colleagues, who described a series of patients with neurologic symptoms associated with low conus and/or thick filum identified on iophenyldate myelography . Previously, this disorder was termed the filum terminale syndrome . Since then, the concept of the tethered cord syndrome has expanded beyond the tight filum and now many of the underlying dysraphic conditions that were excluded by Hoffman and colleagues are considered typical etiologies under the umbrella of tethered cord syndrome .
Siehe auch:
- Spina bifida
- Skoliose
- Cauda equina Lipom
- Syringomyelie
- Myelomeningozele
- Lipomeningomyelozele
- Dysrhaphie
- intradurales spinales Lipom
- normale Position des Conus medullaris Höhe L1 - L2
und weiter:

 Assoziationen und Differentialdiagnosen zu Tethered cord:
Assoziationen und Differentialdiagnosen zu Tethered cord: