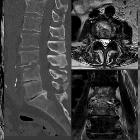
Andersson lesion



An Andersson lesion, also known as rheumatic spondylodiskitis, refer to an inflammatory involvement of the intervertebral discs by spondyloarthritis.
Epidemiology
Rheumatic spondylodiskitis is a non-infectious condition that has been shown to occur in about 8% of patients with ankylosing spondylitis, as detected at radiography.
Pathology
Etiology
There is some debate about etiology. Hypotheses range from spinal (stress) fractures to a local delay in the ankylosing process compared to adjacent levels resulting in the last mobile segment.
Radiographic features
Plain radiograph
Radiography depicts irregularities and erosions of the vertebral endplates that are not related to the anterior or posterior edge but rather to the central portion; such findings are now known to be late features of spondyloarthritis.
MRI
On MR imaging, these lesions are depicted as disc-related signal intensity abnormalities of one or both vertebral halves of a discovertebral unit; they appear hyperintense on STIR images and hypointense on T1-weighted images, where they are often hemispherically shaped. Lines of increased signal intensity may be seen at the interface between the annulus fibrosus and nucleus pulposus or within the latter in early disease.
Just as MR imaging is better than conventional radiography in its depiction of anterior spondylitis (or Romanus lesions), MR imaging also provides a superior view of spondylodiskitis, since the edematous changes in early disease are not radiographically-visualized.
Treatment and prognosis
There is no consensus regarding the management of these lesions and especially when to perform a surgical intervention.
The mainstay of surgical treatment consists of instrumentation and fusion, with correction of kyphotic deformity, if present.
Since radiological appearance, mechanical consequences, prognosis, and management in extensive lesions differ from localized lesions, it has been questioned whether the latter should be classified as Andersson lesions.
Some advocate the eponym "Andersson lesion" to be preserved to extensive lesions, which is actually a spinal pseudarthrosis and the final common pathway of several different etiologies.
History and etymology
The Andersson lesion is named after a Swedish radiologist, Olof Andersson who first described the findings in 1937 whilst working at St Eriks Hospital in Stockholm .
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Andersson-Läsion:
Assoziationen und Differentialdiagnosen zu Andersson-Läsion: