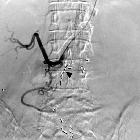
caecal volvulus



















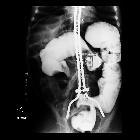



Cecal volvulus describes torsion of the cecum around its mesentery which often results in obstruction. If unrecognised, it can result in bowel perforation and fecal peritonitis.
Epidemiology
Cecal volvulus accounts for ~10% of all intestinal volvuluses, and generally occur in somewhat younger patients than with a sigmoid volvulus, most being 30-60 years old. There are two predisposing factors that are important for the development of a cecal volvulus:
Medical history of these patients may include prior abdominal surgery, the presence of a pelvic mass, violent coughing, atonia of the colon, extreme exertion, unpressurised air travel, or third-trimester pregnancy.
Clinical presentation
Cecal volvulus presents with clinical features of proximal large bowel obstruction. This is usually with colicky abdominal pain, vomiting, and abdominal distension.
Pathology
In ~50% of the patients, the cecum twists in the axial plane, rotating clockwise or counter-clockwise around its long axis and appearing in the right lower quadrant.
The other half of patients have what is known as the loop type of cecal volvulus, in which the cecum both twists and inverts, occupying the left upper quadrant of the abdomen. The terminal ileum is usually twisted along with the cecum. Visualization of a gas-filled appendix confirms the diagnosis.
There is a variant of cecal volvulus termed a "cecal bascule" that occurs when the cecum folds anteriorly without any torsion. A cecal bascule is often seen as a dilated loop in the mid-abdomen and although there is an association with prior surgery, adhesions, and bands they are not essential for a volvulus to occur. In 10% of the population, there is a deficient peritoneal fixation of the cecum and ascending colon allowing abnormal mobility. Depending on the length of the mobile segment of right colon a variety of obstructive bowel patterns may result.
Radiographic features
Two types of cecal volvulus are described although, in practice, the distinction is not clinically relevant:
- axial torsion (described below)
- cecal bascule
Plain radiograph
On abdominal radiographs, there is marked distension of a loop of large bowel with its long axis extending from the right lower quadrant to the epigastrium or left upper quadrant. The general caliber for the cecum is < 9 cm (see the 3-6-9 rule). Depending on the initial bowel position and the length of mobile right colon, the distended cecum may be seen anywhere in the abdomen.
Despite the varying positions of the distended cecum, the plain radiographic features of a cecal volvulus are characteristic, and the caput cecum can typically be identified. The colonic haustral pattern is generally maintained in contradistinction to a sigmoid volvulus although some effacement may be present if ischemia develops. One air-fluid level may be seen in the cecal volvulus in comparison to the sigmoid volvulus with a few air-fluid levels .
When shorter segments of the colon and cecum are involved, the distended cecum may be found in the normal location. In most patients, obstruction is almost complete and the distal colon is usually empty and the small bowel frequently distended.
Fluoroscopy
Contrast enema
A single-contrast barium or a water-soluble contrast enema examination is generally adequate for the evaluation of cecal volvulus. A double-contrast barium enema study does not confer any significant advantage because no fine detail is necessary to make the diagnosis. The administration of glucagon is often necessary because patients may have a considerable colonic spasm and find it difficult to retain the contrast agent.
The barium enema study shows a nondilated distal colon to the point of the twist. If the obstruction is not complete, some barium may trickle past the site of obstruction, and the twist may be visualized in more detail. If the twist occurs along the transverse axis, the obstruction appears relatively smooth, and no spiral twist is usually seen. In a cecal bascule, a rounded termination of the barium column may be seen. This, when seen near a distended gas-filled viscus, should alert the radiologist to the diagnosis of a volvulus.
As little barium as possible should be allowed to flow proximal to the site of obstruction because flooding the bowel proximal to the obstruction site might precipitate a complete obstruction. When the barium enema is administered, overdistension should also be avoided because this can lead to perforation. An attempt should always be made to reduce the volvulus. This reduction may be achieved during colonic filling by barium, but reduction occasionally occurs during barium evacuation. With an intermittent volvulus, the barium enema results may be normal, but a post-evacuation radiograph may reveal the twist.
CT
On axial CT images, cecal volvulus is suggested by the extreme dilatation of the cecum.
When seen on conventional radiographs or tomograms, the cecal volvulus is seen as a rounded focal collection of air-distended bowel with haustral creases in the upper left quadrant.
The two limbs of the looped obstruction gradually taper and converge at the site of the torsion, resulting in the appearance of a bird's beak. This bird beak sign, originally applied to the appearance of sigmoid volvulus on conventional radiographs, can also be appreciated on axial CT images of the loop-type cecal volvulus.
A specific CT sign for volvulus is the whirl sign, which has been described in volvulus of the midgut, cecum, and sigmoid colon . The whirl is composed of spiralled loops of collapsed cecum and sigmoid colon. Low-attenuating fatty mesentery with enhancing engorged vessels radiate from the twisted bowel. In the central eye of the whirl, a soft-tissue density pinpoints the source of the twist. The degree of cecal rotation can even be predicted by the tightness of the whirl.
A recently described sign of a complete volvulus is the X-marks-the-spot sign, referring to the crossing loops of bowel at the site of the transition. Finally, a sign of incomplete or recently resolved complete volvulus is the split wall sign, referring to mesenteric fat seen indenting or invaginating the wall of the bowel.
Treatment and prognosis
Colonoscopic decompression may be appropriate if the patient is unfit for surgery. However, laparotomy is normally required. Where there is colonic ischemia, a right hemicolectomy is performed; in some cases, the primary anastomosis is not possible, and stoma formation at both ends is the safest option.
If the cecum is viable and the volvulus reduces, there are a number of options:
- reduction alone, but this is associated with the highest risk of recurrence
- right hemicolectomy
- cecostomy
- cecopexy
Differential diagnosis
The clinical differential diagnosis is usually between:
- bowel obstruction
- appendicitis
- inflammatory bowel disease
- irritable bowel syndrome
- peptic ulcer disease
To differentiate between sigmoid volvulus and cecal volvulus please refer to Sigmoid volvulus versus cecal volvulus article
See also
Siehe auch:
- Whirlpool-Zeichen
- Dickdarmileus
- mechanischer Ileus
- Sigmavolvulus
- Volvulus
- Magenulkus
- Chronisch-entzündliche Darmerkrankungen
- Appendizitis
- Magenvolvulus
- Zökumperforation
- mobile cecum syndrome
- Cecal bascule
und weiter:

 Assoziationen und Differentialdiagnosen zu Volvulus des Coecums:
Assoziationen und Differentialdiagnosen zu Volvulus des Coecums: