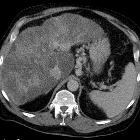
Confluent hepatic fibrosis













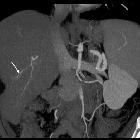












Confluent hepatic fibrosis is a possible result of chronic injury to the liver, most commonly from cirrhosis or hepatic vascular injury.
Radiographic features
Confluent hepatic fibrosis is a cause of wedge-shaped or concave-marginated abnormalities in the cirrhotic liver: it occurs more frequently in the medial and anterior segments of the liver and tends to extend from the hilum to the periphery.
CT
- wedge-shaped regions of hypoattenuation on non-contrast CT
- hypoattenuating on the arterial and portal venous phases
- the fibrosis may gradually enhance
MRI
- wedge-shaped regions of moderate T2 hyperintensity
- T1 hypointensity (possible increased T1 signal from cholestasis)
- progressive postcontrast enhancement on the dynamic sequence but does not show enhancement on the delayed phase with hepatospecific contrast agents
- lack fat signal intensity
Confluent hepatic fibrosis is categorized as LR1 or LR2 in the LI-RADS classification system. If findings are indeterminate between fibrosis and hepatocellular carcinoma, it should be graded LR3 or LR4.
Differential diagnosis
The main differential diagnoses are:
- hepatocellular carcinoma
- enhancement pattern allows differentiation
- not associated with volume loss or capsular retraction
- cholangiocarcinoma
- peripheral cholangiocarcinoma may also show capsular retraction but generally is more masslike
- dilated intrahepatic bile ducts are also more common in cholangiocarcinoma than with confluent hepatic fibrosis
- hepatic epithelioid hemangioendothelioma
- may show capsular retraction but otherwise has a different appearance and enhancement pattern
Practical points
For unknown reasons, confluent fibrosis is more common in primary sclerosing cholangitis and alcohol-related cirrhosis than with viral cirrhosis.
Siehe auch:

 Assoziationen und Differentialdiagnosen zu konfluierende hepatische Fibrose:
Assoziationen und Differentialdiagnosen zu konfluierende hepatische Fibrose: