extradural hematoma vs subdural hematoma




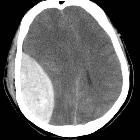





Differentiating extradural (EDH) from subdural (SDH) hemorrhage in the head is usually straightforward, but occasionally it can be challenging. SDHs are more common and there are a few distinguishing features which are usually reliable.
Pathology
History and mechanism of injury
Extradural hematoma
The typical presentation is of a young patient involved in a head strike (either during sport or a result of a motor vehicle accident) who may or may not lose consciousness transiently. Following the injury they regain a normal level of consciousness (lucid interval), but usually have an ongoing and often severe headache. Over the next few hours they gradually lose consciousness.
Subdural hematoma
In adults SDHs are due to falls and there may not be a clear history of trauma. In young children, non accidental injury is a significant cause. The patients level of consciousness gradually decreases with increasing mass effect and confusion is often encountered in the elderly.
Source
Extradural hematoma
Almost always arterial explaining the progressive growth of the hematoma. Classically due to injury of the middle meningeal artery, a branch of the maxillary artery (from the ECA).
Subdural hematoma
Almost always venous due to tearing of subdural cortical bridging veins which extend to the dural sinuses.
Radiographic features
Distribution and appearance
Extradural hematoma
Typically lentiform (lens-shaped, biconvex, lemon-shaped) and do not cross sutures as the periosteum crosses through the suture continuous with the outer periosteal layer.
Subdural hematoma
Typically crescentic (crescent moon-shaped, concave, banana-shaped) and more extensive than EDH, with the internal margin paralleling the cortical margin of the adjacent brain. As these occur in the subdural space, they cross sutures.
Treatment and prognosis
EDH is treated with expedient evacuation via a craniotomy.
SDH has various management strategies depending on the size, location and extent of mass effect and is either conservative (monitor with serial CT) or surgical (drainage with burr holes).
See also
Siehe auch:

 Assoziationen und Differentialdiagnosen zu Unterscheidung epidurales Hämatom subdurales Hämatom:
Assoziationen und Differentialdiagnosen zu Unterscheidung epidurales Hämatom subdurales Hämatom:


