Infarkt des Omentum majus

























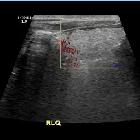





Omental infarction is a rare cause of acute abdomen resulting from vascular compromise of the greater omentum. This condition has a non-specific clinical presentation and is usually managed conservatively. The term along with epiploic appendagitis is grouped under the broader umbrella term intraperitoneal focal fat infarction .
Clinical presentation
Patients may present with :
- sudden onset of abdominal pain
- right lower quadrant pain and tenderness
- absence of fever and gastrointestinal symptoms
- encountered in healthy patients, such as marathoners, because of low omental blood flow
Pathology
Primary omental infarction
The classic location of primary omental infarction is in the right lower quadrant medial to the ascending colon or cecum. The vascular compromise occurs along the right edge of the greater omentum where the arterial supply is usually tenuous.
Sometimes it is the result from kinking of venous channels in the inferior part of the greater omentum in the pelvis. Occasionally omentum twists on itself resulting in omental torsion leading to both arterial and venous compromise. The omentum may infarct without torsion, and this is called primary idiopathic segmental infarction .
Secondary omental infarction
- post surgery
- abdominal trauma
- omental inflammation
Radiographic features
Primary omental infarction is usually seen in the right lower quadrant. Secondary omental infarction is located at the site of initial insult. It is usually larger than 5 cm, which helps distinguishing it from epiploic appendagitis .
Ultrasound
- focal area of increased echogenicity in the omental fat
CT
- focal area of fat stranding
- swirling of omental vessels in omental torsion
- hyperdense peripheral halo
Treatment and prognosis
This condition is often self-limiting and can be managed conservatively. Occasionally complications such as abscess formation occur which require surgery or radiological drainage.
Differential diagnosis
General imaging differential considerations include:
- epiploic appendagitis
- usually smaller areas of fat stranding compared to the omental infarction
- ovoid central area of preserved fat
- hyperdense central dot (thrombosed vessel)
- acute appendicitis
- more a clinical differential, as the appendix should be identified inflamed
- diverticulitis
- fat stranding surrounding a colonic diverticulum
- mesenteric panniculitis
- when differentiating from the omentum, remember that the mesenterium always has a bowel loop at its end
Siehe auch:
- mesenteriale Pannikulitis
- Mesenterialinfarkt
- Omentum
- omental cake
- Appendicitis epiploica
- Divertikulitis
- Appendizitis
- intraperitonealer fokaler lipomatöser Infarkt
- Akutes Abdomen
- peritoneal fat stranding
- Torsion des Omentum majus
- Infarkt Omentum majus bei Kindern
und weiter:

 Assoziationen und Differentialdiagnosen zu Infarkt des Omentum majus:
Assoziationen und Differentialdiagnosen zu Infarkt des Omentum majus:







