Malrotation
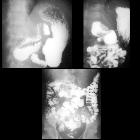
























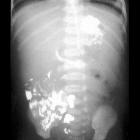



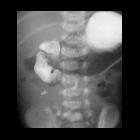







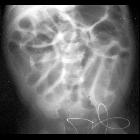











Intestinal malrotation is a congenital anatomical anomaly that results from an abnormal rotation of the gut as it returns to the abdominal cavity during embryogenesis.
Although some individuals live their entire life with malrotated bowel without symptoms, the abnormality does predispose to midgut volvulus and internal hernias, with the potential for life-threatening complications.
Epidemiology
Intestinal malrotation is a congenital abnormality seen in up to 1:6000 live births .
Associations
It is frequently (~50%) associated with other abdominal anomalies, some of which are causative and others merely associated :
- gastrointestinal tract malformations
- duodenal atresia, stenosis or web
- gastroschisis and omphalocele: always associated with a degree of malrotation
- biliary system malformations
- agenesis of the gall bladder
- intra- and extra-hepatic biliary atresia
- pancreatic malformation
- hypoplasia or agenesis of the dorsal pancreas
- congenital diaphragmatic herniation
- heterotaxy: 70% of individuals will have a malrotation
- choanal atresia
- hypospadias
Clinical presentation
The clinical presentation of malrotation often correlates with the age of onset .
In the infant, the most common presentation is with midgut volvulus. Patients with intestinal nonrotation have a lower incidence of midgut volvulus than other types of malrotation.
In the older child or even adult presentation is more frequently intermittent with episodes of spontaneously resolving duodenal obstruction. This is thought to be due to kinking of the duodenum by Ladd bands rather than a volvulus . Internal hernias are also encountered.
In some individuals, the presentation is very non-specific with episodes of abdominal pain, weight loss, melena, or even chronic pancreatitis .
Pathology
During normal embryogenesis, the bowel herniates into the base of the umbilical cord and rapidly elongates. As it returns to the abdominal cavity, it undergoes complex ~270 degrees counter-clockwise rotation resulting in the duodenojejunal (DJ) flexure typically located to the left of the midline, at the level of the L1 vertebral body and the terminal ileum located in the right iliac fossa. This results in a broad mesentery running obliquely down from the DJ flexure to the cecum and prevents rotation around the superior mesenteric artery (SMA) .
In malrotation, this does not occur and, as a result, the mesentery often has a short root, which allows it to act as a pedicle (through which the SMA and SMV pass) around which volvulus can occur.
The rotation of the duodenojejunal loop has been described as beginning around the 5th gestational week and being complete around the 8th. Rotation of the cecocolic loop occurs at a later time, around the 10th week of gestational age. This might explain forms of partial intestinal malrotation .
Intestinal nonrotation is a subtype of malrotation in which the small bowel is mainly located in the right hemiabdomen and the cecum in the left hemiabdomen. The risk of volvulus is much lower in complete nonrotation because patients have the effective anatomy of those who have undergone a Ladd procedure.
Radiographic features
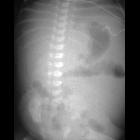
Plain radiograph
Abdominal radiographs, in the absence of midgut volvulus, are neither specific nor sensitive . They may show:
- right sided jejunal markings
- absence of stool filled colon in the right lower quadrant
Ultrasound
May show an inversion in the SMA/SMV relationship with the SMA on the right and the SMV on the left. Although this has classically been advocated as a useful sign for suspecting or excluding intestinal malrotation, a normal SMA/SMV relationship can be seen in up to 29% of patients with surgically proven malrotation, whereas an inverted relationship is seen in up to 11% of patients .
A more useful sign on ultrasound is demonstrating the retro-mesenteric D3 segment of the duodenum, where the horizontal (D3) segment of the duodenum is seen in a transverse plane between the superior mesenteric vessels and the aorta .
Although demonstrating a retro-mesenteric duodenum is extremely sensitive and specific for excluding malrotation, it is not perfect and such a normal anatomic relationship has been described in at least one case of surgically treated intestinal malrotation with midgut volvulus . This case was likely secondary to partial intestinal malrotation, based on the embryological delay described above between the rotation of the duodenojejunal loop and the cecocolic loop.
CT
Depending on the degree of malrotation, CT may show:
- absence of a retro-mesenteric (retro-peritoneal) D3 segment of the duodenum
- may again show abnormal SMA (smaller and more circular)/SMV relationship
- large bowel predominantly on the left and small bowel predominantly on the right
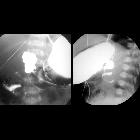
Fluoroscopy
A pediatric upper gastrointestinal contrast study is the examination of choice when the diagnosis is suspected. The key findings of malrotation is an abnormal duodenojejunal (DJ) junction location:
- frontal view
- DJ junction fails to cross the midline to the left of the left-sided vertebral body pedicle
- DJ junction lies inferior to the duodenal bulb
- lateral view
- D2 and D3 segments of the duodenum not located posteriorly in a retroperitoneal position
Although not a specific criteria of malrotation, the jejunum is commonly located to the left of the spine.
Contrast enema has historically also been used, the theory being that in malrotation the large bowel will also be malrotated. Unfortunately, in ~25% (range 20-30%) of cases with malrotation, the cecum is normally located. The converse is also true, with the position of the cecum in normal individuals being variable . Very rarely, the cecum may be malrotated and the small bowel in a normal position.
Treatment and prognosis
Due to the potential for life-threatening midgut volvulus and ischemic bowel, once discovered malrotation is corrected surgically. The general principles of treatment are:
- mobilization of the bowel including untwisting any volvulus present
- division of abnormal peritoneal bands (Ladd bands)
- widening of the mesenteric base
- fixation of the duodenum and cecum to the retroperitoneum (pexy) is not universally performed
- prophylactic appendectomy is often considered, since in later life a delayed/missed diagnosis of appendicitis may occur, due to lack of awareness that the patient has a left sided cecum/appendix causing left sided abdominal pain
It should be noted that normal anatomical positioning is not achieved; the duodenum and small bowel remain on the right, and the cecum and colon are on the left side of the abdomen .
Differential diagnosis
A rate of 15% false positive has been reported in the diagnosis of malrotation using barium meal . Hence, differential diagnoses must be kept in mind, including:
- normal duodenum: located inferiorly because of gastric distension or abnormally because of a feeding tube, renal agenesis, splenomegaly, etc.
- duodenum inversum
- wandering duodenum
Siehe auch:
- Dünndarmileus
- intestinale Malrotation mit Volvulus
- intestinale Malrotation ohne Volvulus
- duodenale Malrotation
- intestinal malrotation and intussusception
- left side appendicitis in midgut malrotation
- midgut nonrotation
und weiter:
- Whirlpool-Zeichen
- Arteria mesenterica superior
- Situs ambiguus
- Duodenalatresie
- normale Darmrotation während der Embrylonalentwicklung
- corkscrew sign
- apple-peel intestinal atresia
- Cornelia-de-Lange-Syndrom
- football sign
- esophageal atresia with H-type tracheo-esophageal fistula
- Polysplenie-Syndrom
- H-type tracheo-oesophageal fistula with no atresia
- McKusick-Kaufman-Syndrom
- neonatal bilious vomiting
- angeborene ösophagotracheale Fistel
- Heterotaxie
- left-sided appendicitis
- jejunoileal atresia
- Malrotation mit Dünndarm-Volvulus
- transverse colon volvulus due to Ladd's band
- intestinale Nonrotation
- delayed gastric emptying in the setting of intestinal malrotation
- malrotation with chronic midgut volvulus
- Ladd's band
- small bowel volvulus due to midgut malrotation
- Malrotation vs. Nonrotation
- asymptomatic intestinal malrotation
- incomplete intestinal malrotation
- Volvulus des Colon transversum
- pediatric cecal malfixation

 Assoziationen und Differentialdiagnosen zu intestinale Malrotation:
Assoziationen und Differentialdiagnosen zu intestinale Malrotation:
