ruptured abdominal aortic aneurysm












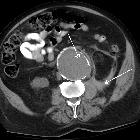










Abdominal aortic aneurysm (AAA) rupture is a feared complication of abdominal aortic aneurysm and is a surgical emergency. It is part of the acute aortic syndrome spectrum.
Epidemiology
Abdominal aortic aneurysms are common and affect ~7.5% of patients aged over 65 years .
Clinical presentation
The classical triad of pain, hypotension, and pulsatile abdominal mass due to rupture into the retroperitoneum is only seen in 25-50% of patients.
A chronic rupture may escape detection for about weeks to months and are known as sealed aneurysmal rupture or spontaneously healed aneurysmal rupture or abdominal aortic aneurysmal leak.
Unusual presentations of ruptured abdominal aortic aneurysm are
- transient lower-limb paralysis
- right upper quadrant pain
- groin pain
- testicular pain
- testicular ecchymosis (blue scrotum sign of Bryant)
- iliofemoral venous thrombosis
Pathology
The aneurysmal rupture is thought to occur when the mechanical stress is in excess of the wall strength. Thus, the aortic aneurysmal wall tension and the aneurysmal diameter are a significant predictor of impending rupture.
The commonest sites of rupture and their relative incidences are
- intraperitoneal rupture: 20%
- retroperitoneal rupture: 80%
- aortocaval fistula: 3-4%
- primary aorto-enteric fistula: < 1%
- aorto-left renal vein fistula: very rare; < 30 cases reported
Radiographic features
Plain radiograph
Abdominal radiographs are not a sensitive mode of detection. A calcified aortic aneurysm may be seen with a secondary blurring of the psoas outline in case of retroperitoneal hemorrhage.
Ultrasound
Not used for routine diagnosis but reported features include.
- focal dilatation of the aorta (aneurysm)
- focal defect at the interface between the vessel lumen and intraluminal thrombus
- sharply demarcated aortic mural defect
- partially detached, mobile layer of intraluminal thrombus
- hypoechoic para-aortic fluid collection
- free intraperitoneal fluid
- heterogenous collection within a retroperitoneal space
- represents retroperitoneal hemorrhage
CT / CT angiography
Retroperitoneal hemorrhage adjacent the aneurysm is the most common finding. The peri-aortic blood may be seen to extend into perirenal or pararenal spaces or the psoas muscles. Intraperitoneal extension of the hemorrhage may be seen as an immediate or a delayed finding.
An important feature seen in contained rupture of an aortic aneurysm is the draped aorta sign - in which the posterior wall of the aorta is not seen distinctly from adjacent structures, and the contour of the aorta follows that of adjacent vertebrae.
A hyperattenuating crescent sign, which is an area of increased attenuation within the aortic aneurysmal mural thrombus, can be demonstrated on plain CT images. This is caused by the insinuation of fresh blood into the mural thrombus and aortic wall.
On post-contrast studies or CT angiography, active extravasation of contrast material can be seen.
Findings predictive of impending rupture
- increased aneurysm size on serial imaging (rate of 10 mm or more per year)
- very large abdominal aortic aneurysm > 7 cm
- reduced thrombus size
- thrombus fissuration
- discontinuity in calcification
- hyperattenuating crescent sign
- well defined peripheral crescent of increased attenuation within the thrombus of a large abdominal aortic aneurysm
Treatment and prognosis
Treatment of an acute rupture should be prompt and can be with endovascular aneurysm repair (EVAR) or open surgery. The mortality rate is very high being > 90% .
Siehe auch:

 Assoziationen und Differentialdiagnosen zu rupturiertes Bauchaortenaneurysma:
Assoziationen und Differentialdiagnosen zu rupturiertes Bauchaortenaneurysma:
