vesico-vaginal fistula
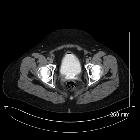

Vesicovaginal fistulas are abnormal fistulous connections between the urinary bladder and vagina, resulting in an involuntary discharge of urine through the vagina.
Epidemiology
The overall incidence of vesicovaginal fistula is unknown but was reported to be 2.11 per 100 births in Nigeria .
Pathology
The tract is lined by squamous epithelium at the vaginal end and transitional epithelium at the bladder end, often with focal ulceration and fibrosis.
Etiology
There are a number of causes including
- prolonged obstructed labor (most common in developing countries)
- surgery, e.g. hysterectomy (most common in developed countries)
- pelvic malignancy (e.g. bladder carcinoma, endometrial carcinoma)
- radiotherapy
- uterine rupture
Other risk factors include trauma, pelvic inflammatory disease and diabetes .
Radiographic features
Cystogram
A fluoroscopic cystogram is a commonly-used method for evaluating this type of fistula. Contrast is injected into the bladder through a Foley catheter and the fistulous tract is outlined. A number of oblique and lateral projections are needed to determine the location.
Gas-fluid levels are seen within the vagina which disappear after 3-4 micturitions, whereas gas bubbles are seen within the bladder for up to one week.
CT
The fistula may be seen as a hypodense area with excretion of contrast into the vagina on delayed CECT images. The tract may be visible if a CT cystogram is performed.
CT, in addition, may provide details regarding the cause of the fistula, such as an adjacent pelvic mass or bowel thickening .
MRI
- T1: tract is centrally hypointense (fluid)
- T2: tract is hyperintense with gas bubbles seen as low signal intensities
- T1 C+ (Gd): peripheral enhancement on contrast
See also
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu vesicovaginal fistula:
Assoziationen und Differentialdiagnosen zu vesicovaginal fistula:


