endometrial carcinoma





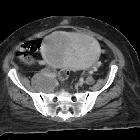
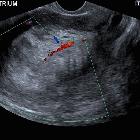





Endometrial carcinoma is generally considered the most common gynecological malignancy. It frequently presents with vaginal bleeding. Both ultrasound and pelvic MRI are useful modalities for evaluation.
Epidemiology
Endometrial carcinoma is the most common gynecological malignancy, with peak incidence at around the 6 decade, though 12% of cases present in premenopausal women. The incidence is thought to be increasing. In the United States, there is a greater incidence among patients of European descent compared those of African American descent.
Clinical presentation
Patients commonly present at an early stage, with postmenopausal bleeding as the initial symptom (present in 90% of patients ).
Pathology
Endometrial carcinoma is divided into two subtypes - type I and type II. The majority are adenocarcinoma.
Type I endometrial carcinoma
Type I (80%) arises in the setting of unopposed hyperestrogenism and endometrial hyperplasia. It is mostly seen in obese women between 55 to 65 years old and is well-differentiated tumor with relatively slow progression and a more favorable outcome . PTEN gene mutation occurs in 30-80% of cases.
Risk factors are anything that leads to increased estrogen exposure:
- estrogen replacement therapy
- polycystic ovarian syndrome and anovulatory cycles
- tamoxifen
- obesity
- early menarche or late menopause
- nulliparity
- estrogen producing ovarian tumors, e.g. granulosa cell cancer
- diabetes mellitus
Type II endometrial carcinoma
Type II (20%) arises in the setting of endometrial atrophy, in females between 65 to 75 years old, and endometrial intraepithelial carcinoma. p53 mutation occurs in up to 50%. This type tends to be less differentiated and spread early via lymphatics or through Fallopian tubes into peritoneum, hence it is associated with a poorer prognosis compared to type I lesions.
Histology
Histological subtypes include:
- type I
- endometrioid carcinoma of the endometrium: commonest histological type: ~85%
- type II
- papillary serous carcinoma of the endometrium: 5-10%
- clear cell carcinoma of the endometrium: 1-5.5%
- adenosquamous carcinoma of the endometrium: ~2%
- adenocarcinoma of the endometrium with squamous differentiation: 0.25-0.50%
- undifferentiated carcinoma of the endometrium
- small-cell undifferentiated carcinoma of the endometrium
Associations
- hereditary non-polyposis colon cancer (HNPCC) : estimated 30-50x increased the lifetime risk
- precursor lesions of complex hyperplasia with atypia are associated with endometrial carcinoma in over 40% of cases
Staging
Most tumors (~80%) present as stage I disease. Endometrial cancer is one of the (less common) causes of cannonball metastases to the lung. See endometrial carcinoma staging for further information.
Radiographic features
Transvaginal ultrasound is the initial imaging investigation of choice for patients presenting with the usual symptom of a postmenopausal bleed. A thickened endometrium requires endometrial sampling.
Staging of endometrial carcinoma is based on the FIGO staging system, which is a surgical and pathological staging following total abdominal hysterectomy, salpingo-oophorectomy, lymphadenectomy, and peritoneal washings. Such radical surgery may not be suitable for elderly patients or those with co-morbidities. MRI has a role in these patients in determining tumor extent and suitable therapy.
Ultrasound
Endometrial carcinoma usually appears as thickening of the endometrium though may appear as a polypoid mass.
- premenopausal: normal endometrial thickness varies through the menstrual cycle
- diagnosing abnormally thickened endometrium depends on knowing what the patient's point in the menstrual cycle
- postmenopausal: >5 mm is thickened (>8 mm if on hormone replacement therapy or tamoxifen)
Sonographic features are non-specific and endometrial thickening can also be due to benign proliferation, endometrial hyperplasia, or polyps. Ultrasound features that are suggestive of endometrial carcinoma rather than hyperplasia include :
- heterogeneous and irregular endometrial thickening
- polypoid mass lesion
- intrauterine fluid collection
- frank myometrial invasion
Disruption of a subendometrial halo on ultrasound may be suggestive of myometrial involvement.
CT
CT has a role in assessing for distant metastases.
Although not generally used for initial diagnosis or local staging, endometrial carcinoma may be encountered on CT:
- non-contrast CT: difficult to differentiate from the normal uterus (especially in local disease)
- post-contrast CT:
- may show diffuse thickening or mass within the endometrial cavity.
- can also have an appearance of a hypo-enhancing and hypo-attenuating mass within endometrial cavity
MRI
A dedicated pelvic MRI protocol is recommended for optimal disease extension assessment and is considered superior to CT for local staging . Contrast-enhanced MRI imaging improves accuracy in detecting myometrial invasion.
- T1: hypo- to isointense to normal endometrium
- T1 C+(Gd)
- carcinomatous tissue will enhance less than normal endometrium
- dynamic contrast-enhanced sequences are good for assessing the depth of myometrial invasion and delayed-phase images cervical stromal invasion
- T2: hyperintense or heterogeneous relative to normal endometrium
- DWI: impeded diffusion, good for assessing the depth of myometrial invasion
FIGO stage
- stage 1: tumor confined to the uterus
- stage 1a: an invasion of less than half of the myometrium
- stage 1b: an invasion of the outer half of myometrium
- stage 2: tumor extends to the cervical stroma
- stage 3: tumor extends beyond the uterus
- stage 3a: tumor invades the serosa or adnexa
- stage 3b: tumor invades the vagina or parametrium
- stage 3c: pelvic/para-aortic lymph node involvement
- 3c1: pelvic lymph node involvement
- 3c2: para-aortic lymph node involvement
- stage 4: bladder/rectal invasion or distant metastases
- stage 4a: tumor extends into adjacent bladder or bowel
- stage 4b: distant metastases
Nuclear medicine
PET-CT is inferior to MRI and ultrasound in the assessment of primary tumors, especially when small or in premenstrual women where there is normally increased physiological endometrial uptake .
Treatment and prognosis
Prognosis depends on various factors including:
- stage: depth of myometrial invasion, lymphovascular invasion, and nodal status
- histological grade
Differential diagnosis
In early disease, the differential is essentially that of endometrial thickening:
- benign endometrial proliferation
- endometrial hyperplasia
- endometrial polyp
- submucosal uterine leiomyoma
Differential considerations for advanced lesions include:
- uterine sarcoma(s)
- uterine lymphoma: rare
- primary uterine lymphoma
- secondary uterine involvement with lymphoma
- cervical cancer with uterine invasion
- metastasis to the uterus from a non-gynecological malignancy: rare
Practical points
- endometrial hyperplasia is a histologic diagnosis, it cannot be differentiated from early-stage endometrial carcinoma
- postmenopausal vaginal bleeding is an important clinical sign for risk stratification of imaging findings
- if present: endometrium >5 mm has 96% sensitivity in the detection of endometrial carcinoma
- if not present: endometrium of >11 mm has been proposed as a threshold for endometrial biopsy
Siehe auch:
- endometrial polyp
- Uterussarkom
- Leiomyofibrom Uterus
- Zervixkarzinom
- endometrial hyperplasia
- maligne Uterustumoren
- endometrial cancer staging
- endometrial stromal sarcoma
- Leiomyosarkom des Uterus
- malignant mixed Mullerian tumour (MMMT) of the uterus
- Lymphom des Uterus
und weiter:
- ovarian thecoma
- cancer
- Adenomyose
- Polyzystisches Ovarialsyndrom
- junctional zone
- polycystic ovaries
- Endometritis
- ovarian fibrothecoma
- hereditary non-polyposis colorectal cancer
- FIGO-Klassifikation
- per vaginal bleeding in the exam
- endometrioid carcinoma of the ovary
- differential diagnosis of an enlarged uterus
- vesico-vaginal fistula
- Granulosazelltumor des Ovars
- PTEN-Hamartom-Tumor-Syndrom
- gynäkologisch radiologisches Curriculum
- ovarian tumours associated with endomterial thickening
- malignant mixed mullerian tumour of the uterus
- clear cell carcinoma of the endometrium
- papillary serous carcinoma of the endometrium
- abnormally thickened endometrium
- undifferentiated carcinoma of the endometrium
- Uteruskarzinom
- tamoxifen associated endometrial changes
- adenosquamous carcinoma of endometrium
- MRT-Protokoll Endometriumkarzinom
- Tamoxifen induzierte Veränderungen des Endometriums
- adenocarcinoma of the endometrium
- endometrioma carcinoma
- Lungenmetastasen bei Endometriumkarzinom
- Rezidiv Endometriumkarzinom
- normale Dicke Endometrium
- Metastasen in der Cervix uteri
- Metastasen Endometriumkarzinom
- endometrial carcinoma: MR findings

 Assoziationen und Differentialdiagnosen zu Endometriumkarzinom:
Assoziationen und Differentialdiagnosen zu Endometriumkarzinom:






