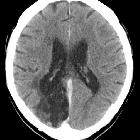
Watershed infarcts











Watershed cerebral infarctions, also known as border zone infarcts, occur at the border between cerebral vascular territories where the tissue is furthest from arterial supply and thus most vulnerable to reductions in perfusion.
Epidemiology
Watershed cerebral infarction account for 5-10% of all cerebral infarctions . They tend to occur in the elderly, who have a higher incidence of arterial stenosis and hypotensive episodes, as well as microemboli.
Pathology
It has been proposed that both episodes of hypoperfusion and microemboli from inflamed atherosclerotic plaques play a role in pathophysiology of this entity, although the latter is less well established .
Episodes of systemic hypotension, particularly with severe stenosis or occlusion of the feeding arteries, in particular the intracranial and extracranial carotid arteries, is the typical scenario in which a watershed infarction is encountered.
Clearance of the microemboli, which may form on the surface of inflamed plaques or are the result of an embolic shower, are most likely to be impaired in watershed zones due to poorer perfusion .
A watershed zone infarct in an isolated area is more likely to be secondary to microembolism, particularly in the absence of significant systemic hypotension and/or arterial stenosis. In a severe carotid stenosis, lesions are usually ipsilateral to the stenosis. Prolonged hypotension, such as during cardiac surgery or cardiac arrest, commonly gives a bilateral pattern in the absence of severe stenosis .
Watershed infarction has been classified as:
- cortical (external) border zones infarct
- between ACA, MCA, and PCA territories
- histologically, these can be wedges of cortical and subcortical infarction or cortical laminar necrosis
- deep (internal) border zones infarct:
- between ACA, MCA, and PCA territories and perforating medullary, lenticulostriate, recurrent artery of Heubner and anterior choroidal arteries
Radiographic features
CT and MRI
The exact pattern depends on the bordering territories, which are usually variable in different individuals. Imaging of watershed infarction should also aim to determine the presence and severity of arterial stenosis and occlusion.
Cortical (external) border zones infarct
These are usually wedge-shaped or gyriform:
- ACA/MCA: in the frontal cortex, extending from the anterior horn to the cortex
- MCA/PCA: in the parieto-occipital region, extending from the posterior horn to the cortex
- parallel parafalcine stripes in the subcortical white matter at the vertex - this type is seen with profound diffuse hypoperfusion
Triple watershed zone: most vulnerable region where ACA, MCA, and PCA converge in the parieto-occipital region posterior to the lateral ventricles.
Deep (internal) border zones infarct
- ≥3 lesions, each ≥3 mm in diameter, in a linear fashion parallel to the lateral ventricles in the centrum semiovale or corona radiata, which sometimes become more confluent and band-like
Siehe auch:

 Assoziationen und Differentialdiagnosen zu Grenzzoneninfarkt:
Assoziationen und Differentialdiagnosen zu Grenzzoneninfarkt: