allergic bronchopulmonary aspergillosis









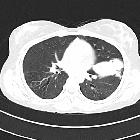


Allergic bronchopulmonary aspergillosis (ABPA) is at the mild end of the spectrum of disease caused by pulmonary aspergillosis and can be classified as an eosinophilic lung disease .
Epidemiology
This entity is most commonly encountered in patients with longstanding asthma, and only occasionally in patients with cystic fibrosis . Only rarely does it appear in patients with no other identifiable pulmonary illness .
In general, patients are young and are diagnosed before the age of 40 years .
Clinical presentation
Clinically, patients have atopic symptoms (especially asthma) and present with recurrent chest infection. They may expectorate orange-colored mucous plugs.
A clinical staging system has been developed:
- stage I: acute
- stage II: remission
- stage III: recurrent exacerbation
- stage IV: steroid-dependent asthma
- stage V: pulmonary fibrosis
Major and minor criteria have also been established .
- major criteria
- clinical
- radiographic features
- pulmonary opacities (transient or chronic)
- central bronchiectasis
- immune system
- blood eosinophilia
- immediate skin reactivity to Aspergillus antigen (elevated IgG and/or IgE against A.fumigatus)
- increased serum IgE (>1000 IU/ml)
- minor criteria
- fungal elements in sputum
- expectoration of brown plugs/flecks
- delayed skin reactivity to fungal antigens
ASPER criteria includes Asthma/atopy history, Serum IgG or IgE against Aspergillus spp., Proximal (central) bronchiectasis, IgE levels >1000ng/mL, and reactive skin test.
Pathology
Allergic bronchopulmonary aspergillosis is the result of hypersensitivity towards Aspergillus spp. which grows within the lumen of the bronchi, without invasion. The hypersensitivity initially causes bronchospasm and bronchial wall edema, which is IgE-mediated. Ultimately, there is bronchial wall damage with loss of muscle and bronchial wall cartilage resulting in bronchiectasis (typically central bronchiectasis) . Both types I and III allergic reactions have been implicated.
Bronchocentric granulomatosis often occurs, which is characterized by necrotizing granulomatous inflammation that destroys the walls of small bronchi and bronchioles. Macroscopically, the mucous plugs are orange/brown in color.
Segmental and subsegmental bronchi are dilated and filled with mucous, admixed with eosinophils and occasional fungal hyphae . Charcot-Leyden crystals may be prominent .
Markers
Laboratory findings include:
- elevated Aspergillus-specific IgE
- elevated precipitating IgG against Aspergillus
- peripheral eosinophilia
- positive skin test
Radiographic features
Plain radiograph
Early in the disease chest x-rays will appear normal, or only demonstrate changes of asthma. Transient patchy areas of consolidation may be evident representing eosinophilic pneumonia.
Eventually, bronchiectasis may be evident. Mucoid impaction in dilated bronchi can appear mass-like or sausage-shaped or branching opacities (finger in glove sign). Pulmonary collapse may be seen as a consequence of endobronchial mucoid impaction.
Fleeting shadows over time can also be a characteristic feature of this disease. These opacities usually appear and disappear in different areas of the lung over a period of time as transient pulmonary infiltrates.
CT
CT findings include:
- fleeting pulmonary alveolar opacities: common
- centrilobular nodules representing dilated and opacified bronchioles
- bronchiectasis
- central, upper lobe saccular bronchiectasis involving segmental and subsegmental bronchi is characteristic
- mucoid impaction results in a bronchocoele, the finger in glove sign
- this may give a Y, V or toothpaste-like configuration
- centrilobular nodular opacities.
- high attenuation mucus +/- (calcification) in impacted mucus in ~30%
- bronchial wall thickening: common
- chronic disease may progress to pulmonary fibrosis, predominantly in the upper lobe
- cavitation: 10%
Treatment and prognosis
Treatment of allergic bronchopulmonary aspergillosis is difficult due to the ubiquity of Aspergillus in the environment. The main focus of treatment revolves around :
- managing asthma
- limiting/controlling exacerbations: corticosteroid plays a major role
- eradicating Aspergillus from the airway: anti-fungal agents, e.g. ketoconazole
- preventing late complications, e.g. severe bronchiectasis, fibrosis
Many patients are successfully managed after diagnosis and never progress clinically to stage IV or V. In stages I to III, prognosis is excellent, whereas stage V has high 5-year mortality from respiratory failure .
Differential diagnosis
For a discussion of the differential diagnosis of bronchiectasis please refer to the article bronchiectasis and more specifically central bronchiectasis.
For mucoid impaction consider:
- mucoid impaction secondary to bronchiectasis
- secondary to an endobronchial lesion
- secondary to atretic bronchial segment
Siehe auch:
und weiter:
- Langerhanszell-Histiozytose der Lunge
- Kartagener-Syndrom
- tree in bud-Muster
- Mukoidimpaktion
- pulmonary opacification
- Bronchialatresie
- primäre ciliäre Dyskinesie
- apical zone
- pulmonale Aspergillose
- PLCH
- Aspergillus fumigatus
- pulmonale Eosinophilie
- aspergillosis
- Thorax Onlinekurs
- Aspergillus clavatus
- Pilzpneumonie
- pulmonary manifestations of cystic fibrosis
- pulmonale Pilzinfektionen
- Aspergillus flavus
- Bronchozele
- bronchiectasis (mnemonic)
- hyperdense Mukusimpaktion
- Finger in Handschuh Bild

 Assoziationen und Differentialdiagnosen zu Allergische bronchopulmonale Aspergillose:
Assoziationen und Differentialdiagnosen zu Allergische bronchopulmonale Aspergillose:

