androgen insensitivity syndrome
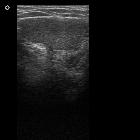



















Androgen insensitivity syndrome (AIS), also known as the testicular feminization syndrome, results from end-organ resistance to androgens, particularly testosterone. AIS may be complete or incomplete with variable imaging findings.
Epidemiology
The incidence may vary depending on whether it is complete or incomplete. Roughly estimated incidence rates are ~1 in 20,000 to 50,000 live births.
Clinical presentation
Patients can often present with primary amenorrhea.
Pathology
Affected individuals are genotypically male with a 46XY karyotype but with a female phenotype (male pseudohermaphroditism). Individuals often have bilateral cryptorchidism. The undescended testes often produce estradiol. There may be a blind-ending vagina.
Genetics
Thought to carry an X linked recessive inheritance where multiple mutations in the androgen receptor (AR) gene has been localized to the long arm of the X chromosome (i.e. Xq11-13).
Subtypes
Although it is a disease spectrum it may be subtyped according to the extent of severity as:
- complete androgen insensitivity syndrome (CAIS): Morris syndrome
- incomplete: partial androgen insensitivity syndrome / Reifenstein syndrome
Radiographic features
General imaging features include:
- bilateral cryptorchidism +/- juxta-testicular Mullerian duct cysts
- absent/rudimentary uterus
- shortened vagina
Ultrasound
Usually, the first modality to locate the testes, and document absent uterus.
MRI
The modality of choice to accurately delineate Mullerian duct anomalies, and localize testes. It may also diagnose testicular malignancy, if any, in cryptorchid testes .
Treatment and prognosis
These patients have an increased incidence of malignancy in the undescended testes:
Differential diagnosis
Mayer-Rokitansky-Kuster-Hauser syndrome has female karyotype with normal female genitalia, and ovaries, but the uterus is rudimentary or absent .
See also
Siehe auch:
- Kryptorchismus
- Seminom
- Zysten des Müller-Gangs
- Mikropenis
- Störungen der geschlechtsspezifischen Entwicklung
- male pseudohermaphroditism
und weiter:

 Assoziationen und Differentialdiagnosen zu Androgenresistenz:
Assoziationen und Differentialdiagnosen zu Androgenresistenz:



