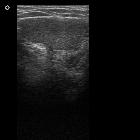
cryptorchidism

















Cryptorchidism refers to an absence of a testis (or testes) in the scrotal sac. It may refer to an undescended testis, ectopic testis, or an atrophic or absent testis. Correct localization of the testes is essential because surgical management varies on location.
Pathology
The testes develop in the abdomen and at ~21 weeks of gestation migrate toward the inguinal canal through the deep inguinal ring. The migration is complete at ~30 weeks. The gubernaculum is the ligament which connects the testes to the scrotum. Under hormonal influence (probably testosterone), the gubernaculum contracts, and the testes descend into the scrotum. Causes/associations of undescended testes are:
- premature birth (birth occurs before full descent of testes)
- intrauterine growth restriction (IUGR)
- associations with smoking, alcohol intake during pregnancy
- androgen insensitivity syndrome
- congenital syndromes
- gestational diabetes
Radiographic features
Ultrasound
Ultrasound has 45% sensitivity, 78% specificity, and 88% accuracy for localization of undescended testis and is more accurate than clinical examination .
- lack of a testicle in the scrotal sac
- the undescended testis is a homogeneously hypoechoic ovoid structure, similar to the contralateral testis, with an echogenic mediastinum testis
- the ectopic testis may be high up in the scrotum or within the inguinal canal (39%)
- ultrasound is limited in intra-abdominal, pelvic or retroperitoneal/ectopic testes (20%)
- ultrasound is also inconclusive in evaluation of the atrophic testis (41%), where it is difficult to differentiate from lymph nodes or the pars infravaginalis gubernaculi
MRI
MRI is the best cross-sectional modality to assess crypto-orchidism (replacing CT). It has a higher sensitivity than ultrasound (~90%) and a higher specificity (100%) .
Coronal T1W images can show the gubernaculum testes and spermatic cord, which can be followed to locate the undescended testes. Also, an ectopic pelvic or retroperitoneal location of testes can be identified. Diffusion-weighted MRI shows the normal testes as markedly hyperintense structures, differentiating them from surrounding structures .
Treatment and prognosis
Most undescended testes at birth descend in the first three months after birth
Orchiopexy is the preferred mode of management in case of viable testes high-up in the scrotum or within inguinal canal/abdomen. It is performed after 1 year of age since the testes may descend without intervention.
With cryptorchidism, there is a 32x increased risk of developing a testicular germ cell tumor, with an incidence of 1 in 2000 (higher in bilateral cases, and in abdominal cryptorchidism) . The effect of surgical correction, decreasing the risk of malignancy is controversial but it does allow for easier examination , and - hopefully - earlier detection.
Differential diagnosis
An exaggerated cremasteric reflex can simulate cryptorchidism.
Siehe auch:
- Androgenresistenz
- Noonan-Syndrom
- Kloakenekstrophie
- Prader-Willi-Syndrom
- Leistenhoden
- Stratton-Parker-Syndrom
- IUGR (Intrauterine growth retardation)
und weiter:
- Eagle-Barrett syndrome
- genitourinary curriculum
- Pätau-Syndrom
- Mikrolithiasis testis
- Ossifizierendes Fibrom
- Beckwith-Wiedemann-Syndrom
- Hoden
- Roberts-Syndrom
- Jaffé-Campanacci-Syndrom
- Ellis-van-Creveld-Syndrom
- Blasenekstrophie
- Tibiale Hemimelie
- Hypospadie
- Cornelia-de-Lange-Syndrom
- Akrorenales Syndrom
- Smith-Lemli-Opitz-Syndrom
- Mammakarzinom beim Mann
- Aarskog-Syndrom
- mesoectodermal dysplasia
- Wolf-Hirschhorn-Syndrom
- Fraser-Syndrom
- acrocephalopolysyndactyly type II
- risk factors for testicular germ cell tumour
- Miller-Dieker Syndrom
- 7-dehydrocholesterol reductase deficiency
- Hypospadia penis
- MEHMO-Syndrom
- Dubowitz-Syndrom
- cryptorchidism with neoplastic transformation (seminoma)

 Assoziationen und Differentialdiagnosen zu Kryptorchismus:
Assoziationen und Differentialdiagnosen zu Kryptorchismus: