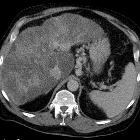
autoimmune hepatitis


Autoimmune hepatitis (AIH) (plural: autoimmune hepatitides) is a rare type of chronic hepatitis, currently classified as "type 1" or "type 2". It may eventually lead to cirrhosis. The role of imaging is primarily to exclude other diagnoses and evaluate for complications.
Epidemiology
It may occur in children or adults, but most patients are affected at 40-60 years old. The incidence in Western Europe is ~0.01-0.02% .
There is no predilection for an ethnic group. There is a female predominance: 3.6: 1.
Clinical presentation
Autoimmune hepatitis has a variable clinical presentation. Patients may be asymptomatic or present in acute liver failure (rare), or anywhere between. It tends to have a relapsing-remitting course. There is an association with other autoimmune conditions.
Depending on the phase, the patient may present with
- hepatomegaly +/- splenomegaly
- jaundice
- elevated aminotransferases (ALT and AST)
Pathology
Autoimmune hepatitis may encompass multiple different conditions.
Type 1:
- "classic" autoimmune hepatitis
- ANA, IgG4, and anti-smooth muscle antibody may be elevated, with the last (1:320) a relatively more specific finding in type 1
- ANCA is more often found in type 1 than in type 2
Type 2:
- has antibodies to liver/kidney microsomes (ALKM-1) or to a liver cytosolic antigen (ALC-1)
Biopsy and histopathology is less specific for a diagnosis, compared to serum markers.
Radiographic features
The role of imaging in a patient with possible autoimmune hepatitis is threefold:
- to exclude other possibilities of chronic hepatitis
- to look for complications of cirrhosis (such as HCC)
- to look for autoimmune involvement of other organs (such as the pancreas).
CT
Non-specific, ranging from normal to hepatomegaly and cirrhosis.
MRI
- T2: non-specific, increased periportal edema
- MRCP: primary sclerosing cholangitis (PSC) should be excluded
Treatment and prognosis
Treatment is similar to other autoimmune conditions, and often uses immunomodulating medications.
Differential diagnosis
- primary biliary cholangitis (PBC)
- primary sclerosing cholangitis (PSC)
- acute hepatitis from other etiologies
- Wilson disease (mostly pediatric patients)
Siehe auch:
- Leberzirrhose
- Primär sklerosierende Cholangitis
- gestational alloimmune liver disease (GALD)
- Autoimmunerkrankungen
- primär biliäre Cholangitis
und weiter:

 Assoziationen und Differentialdiagnosen zu Autoimmunhepatitis:
Assoziationen und Differentialdiagnosen zu Autoimmunhepatitis: