biliary atresia










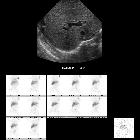
Biliary atresia (BA) is a congenital biliary disorder, which is characterized by an absence or severe deficiency of the extrahepatic biliary tree. It is one of the most common causes of neonatal cholestasis, often causing cirrhosis immediately and leading to death and accounts for over half of children who undergo liver transplantation.
Epidemiology
It is thought to affect 1 in 10,000-15,000 newborn infants. There is a recognized male predilection.
Associations
There are two different forms of biliary atresia (BA):
- non-syndromic BA (~90%): isolated atresia of bile ducts
- syndromic BA (~10%): associated with various congenital anomalies such as polysplenia, asplenia, heterotaxy syndrome, and intestinal malrotation and interrupted IVC
Clinical presentation
It precipitates within the first three months of life. Infants with biliary atresia may appear normal and healthy at birth. Most often, symptoms develop between two weeks to two months of life, and may include:
- jaundice (conjugated hyperbilirubinemia)
- dark yellow or brown urine
- pale or clay-colored (acholic) stools
- hepatomegaly
Complications
Pathology
Etiology
Although typically thought to result from an idiopathic destructive inflammatory process which leads to fibrotic remnants at porta hepatis, the disease may be secondary to viral infections or autoimmune-induced injury in some cases.
Classification
Kasai classification is used to classify the three main anatomical types of biliary atresia.
Radiographic features
Prompt diagnosis ensures early treatment and results in improved prognosis.
Ultrasound
- echogenic fibrous tissue anterior to the portal vein: triangular cord sign
- hepatic artery changes
- larger hepatic arterial caliber
- subcapsular hepatic arterial flow on Doppler
- right proximal hepatic artery diameter >1.5 mm
- hepatic artery to portal vein diameter ratio >0.45
- gallbladder ghost triad
- gallbladder contraction index decreased for the age
Nuclear medicine (hepatobiliary (HIDA) scan)
Tc-99m diosgenin (DISIDA) and mebrofenin (BRIDA) have the highest hepatic extraction rate and shortest transit time of hepatobiliary radiotracers. Cases of biliary atresia typically demonstrate relatively good hepatic uptake with no evidence of excretion into the bowel at 24 hours. Pretreatment with phenobarbital (5 mg/kg/day for 5 days) to increase biliary secretion by stimulating hepatic enzymes is frequently helpful to minimize the possibility of a false-positive study in a patient with a patent biliary system but poor excretion.
Treatment and prognosis
Its important to diagnose it early since Kasai portoenterostomy done within initial 2 months of age has very good prognosis.
Management options include
- Kasai portoenterostomy - the surgery involves exposing the porta hepatis (the area of the liver from which bile should drain) by radical excision of all bile duct tissue up to the liver capsule and attaching a Roux-en-Y loop of jejunum to the exposed liver capsule above the bifurcation of the portal vein creating a portoenterostomy
- liver transplantation
Differential diagnosis
General imaging differential considerations include
- neonatal hepatitis
- Alagille syndrome
- Caroli disease
- bile plug syndrome
- lipid storage disorders
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Gallengangatresie:
Assoziationen und Differentialdiagnosen zu Gallengangatresie:



