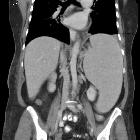
portal hypertension

Caput medusae
bei Pfortaderhochdruck bei Leberzirrhose in der Computertomographie. (sagittal)
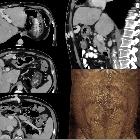
Caput medusae
mit Durchtritt oberhalb des Nabels über Verbindungen der rekanalisierten Nabelvene zu den epigastrischen Gefäßen.

Cirrhosis •
Cirrhosis - Ganzer Fall bei Radiopaedia

Portal
hypertension • Cirrhosis with evidence of portal hypertension - Ganzer Fall bei Radiopaedia

Portal
hypertension • Cirrhosis with portal hypertension - Ganzer Fall bei Radiopaedia

Portal
hypertension • Cirrhosis in a patient with autosomal dominant polycystic kidney disease - Ganzer Fall bei Radiopaedia

Splenomegaly
• Massive splenomegaly - Ganzer Fall bei Radiopaedia

MR imaging in
liver cirrhosis: classical and new approaches. Portal hypertension. MIP vascular image reconstructed from the portal phase shows collaterals vessels and splenomegaly

Portal
hypertension • Hepatic cirrhosis with portal hypertension - Ganzer Fall bei Radiopaedia

Portal
hypertension • Portal venous hypertension - Ganzer Fall bei Radiopaedia

Portal
hypertension • Gastroesophageal varices - Ganzer Fall bei Radiopaedia

Portal
hypertension • Distal intestinal obstruction syndrome and cirrhosis - Ganzer Fall bei Radiopaedia

Portal
hypertension • Enlarged paraumbilical vein - Ganzer Fall bei Radiopaedia

Hepatofugal
flow in portal vein in ultrasound - patient has known cirrhosis

Großkalibrige
portosystemische Umgehungskreisläufe über Venen der Bauchwand. Computertomographie: Rekonstruktion mit Volume-rendering-Technik

Großkalibrige
portosystemische Umgehungskreisläufe über Venen der Bauchwand. Computertomographie: Rekonstruktion mit Volume-rendering-Technik

Großkalibrige
portosystemische Umgehungskreisläufe über Venen der Bauchwand. Computertomographie: Rekonstruktion mit Volume-rendering-Technik
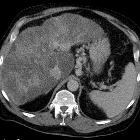
Fundusvarizen
bei Leberzirrhose mit portaler Hypertension. Computertomographie axial.

Caput medusae
bei Pfortaderhochdruck bei Leberzirrhose in der Computertomographie. (axial)

Toddler with
cavernous transformation of the portal vein. AP (left) and lateral (right) images of the esophagus from an upper GI exam show multiple longitudinal luminal filling defects in the distal esophagus representing esophageal varices.The diagnosis was esophageal varies due to portal hypertension.
Portal hypertension is defined as hepatic venous pressure gradient (HVPG) greater than 5 mmHg. HVPG is a surrogate for the portosystemic pressure gradient. Clinically significant portal hypertension is defined as a gradient greater than 10 mmHg and variceal bleeding may occur at a gradient greater than 12 mmHg.
Pathology
Causes can be split by their relation to the hepatic sinusoids:
Prehepatic causes
- portal vein thrombosis
- extrinsic compression of portal vein
- congenital portal vein stenosis
- arteriovenous fistula
- SVC obstruction (downhill varices)
Hepatic / sinusoidal causes
- cirrhosis
- viral hepatitis
- Schistosomiasis (S. mansoni or S. japonicum)
- congenital hepatic fibrosis
- infiltrative liver diseases
- polycystic liver disease
- nodular regenerative hyperplasia
- idiopathic portal hypertension
Posthepatic causes
- Budd-Chiari syndrome
- sinusoidal obstruction syndrome
- congestive cardiac failure
- constrictive pericarditis
Subtypes
Radiographic features
Ultrasound
- dilated portal vein (>13 mm): non-specific
- biphasic or reverse flow in portal vein (late stage): pathognomonic
- recanalization of paraumbilical vein: pathognomonic
- portal-systemic collateral pathways (collateral vessels/varices)
- splenomegaly
- ascites
- cause of portal hypertension often identified, most commonly cirrhosis
CT and MRI
- dilated portal vein +/- mesenteric veins
- contrast enhancement of paraumbilical vein: pathognomonic
- collateral vessels/varices: these are many and can include
- coronary venous collaterals: considered one of the commonest
- esophageal collaterals
- paraumbilical collaterals
- abdominal wall collaterals
- perisplenic collaterals
- retrogastric collaterals
- paraesophageal collaterals
- omental collaterals
- retroperitoneal collaterals
- mesenteric collaterals
- splenorenal collaterals
- gastrorenal collaterals
- splenomegaly
- ascites
- cause of portal hypertension often identified, most commonly liver cirrhosis
Treatment and prognosis
- dietary restriction
- medication: propranolol, diuretics
- interventional procedures
- transjugular intrahepatic portosystemic shunt (TIPS)
- surgical portosystemic shunt
- surgical splenorenal shunt
- balloon dilatation of hepatic vein (in case of thrombosis/web in hepatic vein)
- transhepatic clot thrombolysis (in portal vein thrombosis)
- splenic artery embolization
- liver transplantation
- treatment of complications
Complications
- ascites
- esophageal varices and gastric varices
- variceal bleeding (30-50% mortality with each bleed)
- portal hypertensive gastropathy/enteropathy/colopathy
- hepatic encephalopathy
- hepatorenal syndrome
- hepatopulmonary syndrome
- congestive splenomegaly and hypersplenism
Differential diagnosis
Dilatation of splenic veins at the splenic hilum without splenomegaly may occur in situations such as state of increased perfusion of splenic tissue associated with an immune response .
Siehe auch:
- Leberzirrhose
- Splenomegalie
- Pfortaderthrombose
- portosystemische Umgehungskreisläufe
- Aszites
- transjugulärer intrahepatischer portosystemischer Shunt
- Budd-Chiari-Syndrom
- Hepatische Enzephalopathie
- Cruveilhier-Baumgarten-Syndrom
- Venenverschlusskrankheit der Leber
- portal-hypertensive Gastropathie
und weiter:
- kavernöse Transformation Pfortader
- Morbus Osler-Weber-Rendu
- Gamna-Gandy Körperchen
- hepatopetal
- Caput medusae
- Caput medusae Zeichen bei DVA (developmental venous anomaly)
- Ösophagusvarizen
- erweiterte Vena azygos
- Milzarterienaneurysma
- COACH syndrome
- Arterielle Hypertonie
- portale Biliopathie
- Fundusvarizen
- Echinokokkose der Milz
- hepatofugaler Fluss in der Vena portae
- diffuse mesenteriale Flüssigkeitseinlagerungen (misty mesentery sign)
- Wassermelonenmagen
- duodenal varices
- pathological conditions of hepatic vascularization
- Hypertonus
- abdominelle Manifestationen bei Mukoviszidose
- Varizen der Vena mesenterica superior
- portalvenöse Verkalkungen
- portopulmonale Hypertension
- Sichelzellenanämie (abdominelle Manifestationen)
- enlarged azygos vein from portal hypertension
- high signal intensity in the basal ganglia in portal hypertension
- splenic varices
- Zökumvarizen
- Varizen der Vena renalis

 Assoziationen und Differentialdiagnosen zu portale Hypertension:
Assoziationen und Differentialdiagnosen zu portale Hypertension:transjugulärer
intrahepatischer portosystemischer Shunt