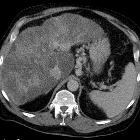
Esophageal varix














Esophageal varices describe dilated submucosal veins of the esophagus, and are an important portosystemic collateral pathway. They are considered distinct from gastric varices, which are less common.
Epidemiology
Esophageal varices are present in ~50% of patients with portal hypertension . They occur in greater frequency in patients with more severe cirrhosis, for example esophageal varices may be present in ~40% of patients with Child-Pugh A, but in ~85% of patients with Child-Pugh C cirrhosis .
Clinical presentation
Patients will generally be asymptomatic until a variceal hemorrhage, which occur at a yearly rate of 5-15% . In the case of a variceal bleed, patients will usually present with stigmata of upper gastrointestinal bleeding, such as hematemesis, melena, presyncope and syncope, and progression to hypovolemic shock . The primary predictor of variceal bleed is variceal wall tension, which is a metric that encompasses vessel diameter (larger is worse) and pressure (higher is worse) .
Additionally, patients will often have stigmata of portal hypertension and cirrhosis – the most common etiological basis for esophageal varices.
Pathology
Two types of esophageal varices have been described.
- uphill esophageal varices
- most common form
- typically caused by portal hypertension, as a collateral pathway between the portal vein and the superior vena cava (via the azygos vein)
- the most common cause of this phenomenon is cirrhosis , however less common non-cirrhotic etiologies include primary biliary cirrhosis, primary sclerosing cholangitis, portal vein thrombosis, Budd-Chiari syndrome, and schistosomiasis
- typically present in the lower third of the esophagus
- commonly co-occur with gastric varices, which have an identical pathophysiology, but are notably less common
- when co-occurring, most commonly there is extension of the esophageal varices along the lesser curvature of the stomach (Type GOV1 in the Sarin classification)
- may be associated with paraesophageal varices, which are varices of the adventitial esophageal veins, and confer a low bleeding risk
- downhill esophageal varices
- relatively rare
- typically caused by superior vena cava obstruction, as part of superior vena cava syndrome, as a collateral pathway between the superior vena cava into the portal circulation and/or the inferior vena cava
- typically present in the upper third of the esophagus, although can span the entire esophagus if the superior vena cava obstruction is proximal to the inflow of the azygos vein
- do not co-occur with gastric varices due to a different pathophysiological basis
- have a relatively lower bleeding risk
Radiographic features
The gold-standard investigation for the evaluation of esophageal varices is esophagogastroduodenoscopy, however radiographic investigations may serve as a useful non-invasive adjunct.
Plain radiograph
Esophageal varices may be visible on plain radiograph if they are large. In such instances, they will have a non-specific appearance of a mass in the posterior mediastinum .
Fluoroscopy
Barium swallow may reveal longitudinal esophageal luminal filling defects, representing esophageal varices .
CT/MRI
Esophageal and paraesophageal varices are readily visible on contrast-enhanced cross-sectional imaging, as torturous, enlarged, smooth enhancing tubular structures . They, depending on size and pressure, may protrude into the esophageal lumen . In association, the esophageal wall is also often thickened .
DSA
Digital subtraction angiography can also be a useful imaging modality in the assessment of esophageal and paraesophageal varices, providing direct visualization through catheterization and contrast injection of the left gastric vein . However, smaller varices are often not appreciated .
Treatment and prognosis
The mainstay of management for uphill esophageal varices is primary prevention, which can be pharmacological (typically with non-selective beta-blockers), or with invasive endoscopic variceal ligation . The decision between pharmacological or endoscopic prevention is rather complex, and depends on factors such as variceal size and severity of cirrhosis . In patients with a prior variceal hemorrhage, the focus of management is secondary prevention, which can again be pharmacological (typically with non-selective beta-blockers), with invasive endoscopic variceal ligation, or through surgical creation of a portosystemic shunt (e.g. transjugular intrahepatic portosystemic shunt) .
In the event of acute variceal hemorrhage, management includes resuscitation with intravenous fluids and blood products, administration of vasoactive drugs (such as terlipressin or octreotide), intravenous antibiotics, and endoscopic ligation . In severe cases refractory to standard management, salvage therapy with a Sengstaken-Blakemore tube or a Minnesota tube can be attempted .
The management of downhill esophageal varices is quite different, and the focus is on treating the cause of the superior vena cava obstruction . Unlike uphill esophageal varices, beta-blockade may not be useful, however endoscopic variceal ligation or banding may be appropriate .
See also
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Ösophagusvarizen:
Assoziationen und Differentialdiagnosen zu Ösophagusvarizen: