clavicular fracture



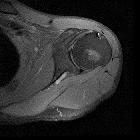















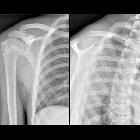
Clavicular fractures are common and account for ~5% (range 2.6-10%) of all fractures . They usually require minimal treatment, which relies on analgesia and a collar-and-cuff. However, in some cases, open reduction and internal fixation are required.
Epidemiology
Clavicular fractures are most common in young adults and elderly women .
Risk factors
- osteoporosis (for elderly women)
Pathology
Fractures can occur at any part of the clavicle. However, the vast majority (~75%; range 69-85%) occur in the midshaft, at or near the junction of the middle and outer third with distal clavicle fractures (15-20%) and medial clavicle fractures (<5%) less common .
Bipolar clavicular fractures occur when there are both distal and medial clavicular injuries, most commonly a distal clavicle fracture in combination with an anterior sternoclavicular joint dislocation .
Mechanism
Typically, fractured clavicles occur as the result of a direct blow to the shoulder. Fall onto the shoulder or onto an outstretched arm can cause this.
The midshaft fracture dominance is due to two factors: firstly this is the thinnest part of the bone, and secondly, it is the only part of the bone not reinforced by attached musculature and ligaments .
Classification
- Neer classification of clavicle fractures
- AO classification of clavicle fractures
Radiographic features
Plain radiograph
While it is not unusual for only a single AP film to be obtained, ideally, as with any trauma situation, two views are better than one. In most trauma situations, orthogonal views of the affected bone or joint are obtained. Since this is not possible with the clavicle, AP and axial views are obtained:
In most instances, the fracture is evident clinically and easily identified on radiographs. It is common for clavicle fractures to be displaced due to a combination of the weight of the upper limb pulling the distal fragment down and the sternocleidomastoid pulling the medial fragment upwards.
It is important to note that occult fractures may be present in the apparently normal radiograph; this is relatively common in children and also occasionally seen in adults .
Radiology report
Radiology reports should not only include whether or not a fracture is present but also comment on:
- fracture
- location of the fracture along the shaft
- angulation and fracture end displacement (including direction)
- comminution
- degree of overlap (measurement is useful)
- associated findings and relevant negatives
- acromioclavicular joint and sternoclavicular joint alignment
- coracoclavicular distance
- glenohumeral joint
- associated traumatic injuries
- rib fractures
- vertebral fractures
- scapular fractures (floating shoulder)
- pneumothorax
Treatment and prognosis
In cases where the clavicle is thought to be fractured clinically, but where the radiograph is normal, it is advisable to treat patients as if a fracture is present; this is especially the case in children .
Traditionally midshaft fractures of the clavicle have been treated with immobilization and a sling or figure-of-8 dressing, and in most cases, results are said to be excellent with low non-union rates and minimal functional impairment . This has been challenged by some authors, who have found non-union rates of up to 15% and high rates of a suboptimal outcome, e.g. ongoing local pain, brachial plexus irritation, cosmetic deformity .
In cases where there is significant displacement, angulation, shortening (>2 cm) or comminution, internal fixation either with plate-and-screw fixation or with a medullary device (e.g. intramedullary titanium elastic nail) has shown to result in a better cosmetic outcome and higher rates of union. Internal fixation is thus probably advisable in such cases and in patients who are at risk of non-union (e.g. elderly) .
Additionally, cosmetic concerns may be an indication of internal fixation to avoid unsightly deformity.
For unstable distal clavicular fractures, a coracoclavicular screw fixation could be performed.
Siehe auch:
- AO Klassifikation Klavikulafraktur
- Musculus sternocleidomastoideus
- Frakturen der oberen Extremitäten
- Klassifikation laterale Klavikulafraktur nach Jäger und Breitner
- laterale Klavikulafraktur
- Morbus Friedrich
- AO-Klassifikation
und weiter:
- Prévot-Nagel
- Schulterluxation
- proximale Humerusfrakturen
- Luxation Sternoklavikulargelenk
- Klavikula
- clavicle fracture complicating into pyopneumothorax and non union
- Edinburgh-Klassifikation laterale Klavikulafraktur
- Claviculafraktur Einteilung
- outer third clavicle fractures
- mittlere Klavikulafraktur
- birth trauma (physical)
- clavicular fracture non union
- Klassifikation laterale Klavikulafraktur nach Neer
- clavicle greenstick fracture
- Prinzipien nach Goss laterale Klavikulafraktur
- Einteilung distale Klavikulafraktur
- segmental fracture of the clavicle
- fracture of the medial third of the clavicle
- bilateral clavicle fractures

 Assoziationen und Differentialdiagnosen zu Klavikulafraktur:
Assoziationen und Differentialdiagnosen zu Klavikulafraktur:
