deep vein thrombosis










Deep vein thrombosis (DVT) most commonly occurs in the lower limbs, however, are not uncommon in the upper limb and neck veins. Other types of venous thrombosis, such as intra-abdominal and intracranial, are discussed in separate articles.
Terminology
The term indeterminate (equivocal) DVT is preferred over subacute DVT when the ultrasound features are of neither acute DVT nor chronic post-thrombotic change (although subacute DVT can be used in the follow-up of a known acute DVT). The term chronic post-thrombotic change is preferred over chronic or residual DVT to prevent overtreatment with anticoagulation .
Epidemiology
- 1.6 new cases per 1000 per year
- 2.5-5% of the population is affected
- >50% have long terms symptoms of post-thrombotic syndrome
- 6% of DVT patients report eventual venous ulcers (0.1% general population)
Risk factors
- age (relative risk increase ~2 per 10-year increase)
- surgery (orthopedic patients at highest risk: hip 48%, knee 61%)
- trauma
- history of venous thromboembolism (2-9% increase)
- primary hypercoagulable states
- protein A, C, and S deficiency (10 x increased risk)
- factor V Leiden (heterozygous 8 x increased risk, homozygous 80x)
- estrogen replacement (2-4 x increased risk)
- immobilization (2 x increased risk)
- pregnancy (0.075% of pregnancies)
- greatest risk is in the postpartum period, risk returns to baseline 6 weeks after delivery
- malignancy (4-6 x increased risk)
- in-dwelling vascular device (e.g. PICC line and upper limb DVT)
Clinical presentation
In the lower limbs, patients often present with unilateral leg pain, swelling, and erythema. On physical examination, the affected leg is often tender and warm, and there may be dilation of superficial veins. Additionally, some patients may have a positive Homan sign on physical examination, whereby there is pain on forceful dorsiflexion while the knee is extended.
The Wells score for DVT, a clinical decision rule, can help to stratify risk in patients presenting with symptoms of acute DVT .
Pathology
The majority of DVTs occur in the lower extremities and begin in the soleal veins of the calf.
Markers
In patients deemed to "unlikely" have a DVT via the Wells score, a negative d-dimer can safely exclude acute DVT .
Radiographic features
Complete duplex ultrasound is the imaging modality of choice .
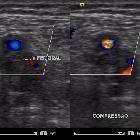
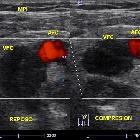
Ultrasound
- general features
- non-compressible venous segment
- loss of phasic flow on Valsalva maneuver
- absent color flow if completely occlusive
- lack of flow augmentation with calf squeeze
- increased flow in superficial veins
- acute thrombus
- increased venous diameter
- soft/deformable intraluminal material
- smooth surface
- free-floating edge (uncommon)
- chronic post-thrombotic change
- normal or decreased venous diameter
- rigid intraluminal material
- irregular surface
- synechiae or bands
- calcifications (rare)
- +/- acute thrombus
MRI
Vascular structures should always be interrogated during routine assessment of the peripheries and pelvis. Incidental DVT has a prevalence of around 0.3% on routine outpatient knee MRI :
- luminal abnormalities (abnormal flow voids or filling defects)
- vein wall thickening
- perivascular edema
- perifascial edema
- local intramuscular T2/PD hyperintensity
- subcutaneous edema
- dermal thickening (related to venous obstruction)
Treatment and prognosis
Treatment is with anticoagulation, often for at least 3 months in duration .
Complications
Practical points
- "above knee DVT", or proximal DVT, is a lower limb DVT involving the popliteal vein or more proximal vessels
Siehe auch:
- Lungenarterienembolie
- Kollateralvenen
- venous thromboembolism
- venöse Verkalkungen
- oberflächliche Venenthrombose
- Phlebothrombose
- Thromboseprophylaxe
- postthrombotisches Syndrom
und weiter:

 Assoziationen und Differentialdiagnosen zu tiefe Venenthrombose:
Assoziationen und Differentialdiagnosen zu tiefe Venenthrombose:



