haemolytic anaemia
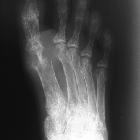
Hemolytic
anemia • Hemolytic anemia with secondary gout - Ganzer Fall bei Radiopaedia

Hemolytic
anemia • Autoimmune hemolytic anemia - Ganzer Fall bei Radiopaedia
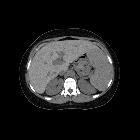
Teenager with
autoimmune hemolytic anemia who has had multiple blood transfusions. Axial CT without contrast of the abdomen shows a marked homogeneous increase in liver density which is making the portal veins and hepatic veins appear to be low attenuation in comparison to the liver.The diagnosis was hemosiderosis.
Hemolytic anemia is a form of anemia where red blood cells are destroyed faster than they can be replaced. This may happen either intravascularly or extravascularly.
Clinical presentation
The patient presents with anemia and jaundice. Diagnosis is based on several laboratory parameters:
- reticulocytosis
- suggested by a raised mean cell volume (MCV)
- a blood film can confirm
- increased unconjugated bilirubin
- increased lactate dehydrogenase
- decreased haptoglobin
Pathology
With the excessive red cell destruction, there is compensatory erythroid hyperplasia in the bone marrow, resulting in increased production of erythroid precursors (reticulocytosis).
Causes
Hereditary
Hemolytic anemia can be due to defects in:
- metabolism
- red blood cell membrane production
- hereditary spherocytosis
- hereditary elliptocytosis
- hemoglobin production
Acquired
- autoimmune diseases
- systemic lupus erythematosus
- rheumatoid arthritis
- infection
- viral
- mycoplasma
- lymphoproliferative disorder
- portal hypertension (resulting in hypersplenism)
- paroxysmal nocturnal hemoglobinuria (PNH)
- drug-induced
- phenacetin
- quinidine
- alpha-methyldopa
- lead poisoning
- secondary to malignancy
- prosthetic heart valves: primarily due to mechanical trauma of the RBCs
Radiographic features
Chronic hemolytic anemia may present on imaging as marrow reconversion and/or splenomegaly. Some underlying causes of hemolytic anemia (e.g. sickle cell disease) have more specific imaging findings: see the relevant articles for more details.
Siehe auch:

