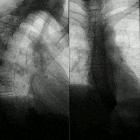
systemic lupus erythematosus
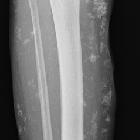














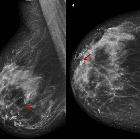

Systemic lupus erythematosus (SLE) is a complex autoimmune disease with multisystem involvement. Although abnormalities in almost every aspect of the immune system have been found, the key defect is thought to result from a loss of self-tolerance to autoantigens.
Epidemiology
There is a strong female predilection in adults, with women affected 9-13 times more than males. In children, this ratio is reversed, and males are affected two to three times more often.
While it can affect any age group, the peak age at onset around the 2 to 4decades, with 65% of patients presenting between the ages of 16 and 65 years (i.e. during childbearing years). The disease is sometimes classified according to early and late-onset groups.
Prevalence varies according to ethnicity with ratios as high as 1:500 to 1:1000 in Afro-Caribbeans and indigenous Australians, down to 1:2000 in Caucasians .
Pathology
SLE can affect multiple components of the immune system, including the complement system, T-suppressor cells, and cytokine production. Emerging evidence has demonstrated a key player in the generation of autoantigens in SLE is the increase in generation (i.e. increased apoptosis) and/or decrease in clearance of apoptotic cell materials (i.e., decreased phagocytosis). It can result in generation of autoantibodies, which may circulate for many years prior to the development of overt clinical SLE. The disease tends to have a relapsing and remitting course.
SLE has a myriad of clinical features and radiographic presentations that are discussed under individual subtopics:
- CNS manifestations of systemic lupus erythematosus (CNS lupus): neuropsychiatric events can occur in ~45% (range 14-75%) of cases
- gastrointestinal manifestations of systemic lupus erythematosus: there may be GI involvement in ~20% of cases
- musculoskeletal manifestations of systemic lupus erythematosus
- renal manifestations of systemic lupus erythematosus
- thoracic manifestations of systemic lupus erythematosus
Genetics
Though the pathogenesis of SLE is complex and not yet completely understood, there is a known genetic predisposition with multiple twin studies demonstrating higher concordance in monozygotic twins . Susceptibility likely results from a combination of multiple genetic and epigenetic aberrations with over 60 risk loci identified. Changes in gene expression contributing to SLE can be due to any and all of the sequence mutation, DNA methylation, histone modification, miRNAs and lncRNAs .
Environmental factors
Ultraviolet light (increased keratinocyte apoptosis), infection (via molecular mimicry and bacterial CpG motifs), smoking (odds ratio (OR): 1.56 in current smokers, 1.23 in ex-smokers), environmental pollutants (silica) and intestinal dysbiosis are all known risk factors for SLE.
A number of culprit drugs have been involved in the development of drug-induced lupus which is a similar but separate disease entity characterized by generation of anti-dsDNA and anti-histone antibodies and a more protracted disease course resolving with withdrawal of the causative medicine. Drugs include chlorpromazine, diltiazem, hydralazine, IFN-alpha, isoniazid, methyldopa, minocycline, penicillamine, procainamide, quinidine.
TNF inhibitors can similarly induce autoantibodies in up to 70-80% of patients but rarely causes clinical lupus.
Markers
Almost all patients with SLE have a positive ANA (NPV >99%). Approximately 85% (range 70-98%) of patients test positive for anti-dsDNA antibodies , which can also be used to monitor disease activity. ~20% of Caucasians and ~35% of Asians/blacks test positive for anti-Smith antibodies which are highly specific for SLE and tend to indicate a more serious disease course with renal and CNS involvement. Other antibodies (and associations) include anti-Ro (neonatal lupus, subacute cutaneous lupus, secondary Sjögren syndrome), anti-La (neonatal lupus, secondary Sjögren syndrome), anti-U1 RNP (myositis, secondary Raynaud phenomenon), anti-ribosomal P (neuropsychiatric manifestations). Low complement C3 and C4 levels are often seen, especially during flares and active disease.
Diagnosis
The diagnosis of SLE may be made be if four of eleven ACR (American College of Rheumatology) criteria are present, either serially or simultaneously . These criteria were initially published in 1982 but were revised in 1997.
ACR criteria:
- malar rash: fixed, flat or raised, occurs over malar eminences and tends to spare the nasolabial folds.
- discoid rash: erythematous raised patches with adherent keratotic scaling and follicular plugging
- photosensitivity
- oral ulcers
- non-erosive arthritis: where there is involvement of two or more peripheral joints with tenderness, swelling or joint effusions; can occur in ~80% of cases
- pleuritis and/or pericarditis: present in ~35% (range 17-50%) of cases
- proteinuria: >0.5 g/day
- hematological abnormality
- hemolytic anemia or
- leukopenia: <4000/mm on more than two occasions
- lymphopenia: <1500/mm on more than two occasions
- thrombocytopenia: <100,000/mmwithout any precipitant medications
- neuropsychiatric manifestations
- seizures or psychotic events in the absence of any underlying precipitating drugs or metabolic abnormalities
- immune abnormality on serology
- anti-DNA antibodies or
- anti-Sm antibodies or
- antiphospholipid antibodies (requires certain criteria)
- 27-42% of SLE patient can have antiphospholipid antibody syndrome
- positive antinuclear antibodies
Treatment and prognosis
Recent advances in diagnosis and treatment strategies has resulted in a survival improvement from 5-year survival at 40-50% in the 1950s up to a 10-year survival now estimated at 80-90%. Nevertheless, patients with SLE have a standardized mortality ratio of 3. Early deaths in disease course are usually due to active disease and immunosuppression while late deaths tend to arise from coronary artery disease and SLE or treatment complications (e.g. end-stage kidney disease from lupus nephritis) .
History and etymology
Lupus is the Latin word for 'wolf'. Historically there were physicians who believed certain dermatological manifestations associated with the disease appeared similar to wolf bites , however, they did not necessarily understand the disease modern physicians do. The modern understanding of the disease began with the work of Moritz Kaposi in the late 1800s.
Siehe auch:
- Vaskulitis
- Systemische Sklerodermie
- subkutane Verkalkungen
- Lupus erythematodes ZNS
- muskuloskelettale Manifestationen systemischer Lupus erythematodes
- Lupus erythematodes Niere
- systemic lupus erythematosus of myelon
und weiter:
- Rippenusuren
- verkalkte Milzläsionen
- Aneurysma spurium
- Polyarteriitis nodosa
- Sklerodermie Ösophagus
- multiple Milzverkalkungen
- Pleuraempyem
- Splenomegalie
- Thymom
- inflammatorischer Pseudotumor der Orbita
- zystische Lymphknoten
- Ileitis terminalis
- Thymuskarzinom
- Aortitis
- Patellarsehnenruptur
- Nierenvenenthrombose
- Kardiomegalie
- Moyamoya-Erkrankung
- Neuritis nervi optici
- lymphozytisch interstitielle Pneumonie
- posteriores reversibles Enzephalopathiesyndrom
- Achillessehnenruptur
- posttraumatisches Aneurysma spurium
- FCE
- Thymushyperplasie
- Interstitielle Lungenerkrankung
- Quadrizeps-Sehnenruptur
- radiologisches muskuloskelettales Curriculum
- causes of pulmonary arterial hypertension
- interstitial pneumonia
- mixed connective tissue disease
- Autosplenektomie
- Jaccoud-Arthropathie
- fibrosierende Mediastinitis
- bilaterale axilläre Lymphadenopathie
- pulmonary manifestations of scleroderma
- invasives Thymom
- stroke in children and young adults
- Pneumonitis
- Kikuchi-Fujimoto disease
- Winiwater-Buerger-Krankheit
- small fiber neuropathy
- differential diagnosis of intramuscular high STIR signal on MRI
- Rheuma Differentialdiagnose
- Chorea
- musculoskeletal manifestations of AIDS
- Muskelödem
- dystrophic calcification within the breast
- diffuse Alveolarblutung
- retinocochleocerebral vasculopathy
- temporomandibular joint inflammation
- dens erosion
- Raynaud-Syndrom
- thymic epithelial tumours
- focal splenic calcifications
- Bazex-Syndrom
- lupus cerebritis
- neuropsychiatric systemic lupus erythematosus
- sjögren syndrome associated with systemic lupus erythematosus
- gastrointestinale Vaskulitis bei systemischem Lupus Erythematodes
- SLE-Sjögren overlap syndrome
- muskuloskelettale Manifestationen rheumatoide Arthritis
- Weichteilverkalkungen bei systemischem Lupus Erythematodes
- chronische Periaortitis

 Assoziationen und Differentialdiagnosen zu systemischer Lupus Erythematodes:
Assoziationen und Differentialdiagnosen zu systemischer Lupus Erythematodes: