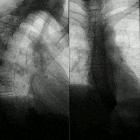
pulmonary manifestations of scleroderma




Pulmonary manifestations of scleroderma are demonstrated histologically in 90% of patients with scleroderma. It is a leading cause of mortality and at autopsy. The lung is reportedly involved in close to 100% of cases. However, only 25% of patients will present with respiratory symptoms or demonstrate abnormalities on CT .
For a discussion of scleroderma in general, refer to parent article: scleroderma.
Clinical presentation
In patients who are symptomatic due to pulmonary involvement, respiratory function tests typically demonstrate a restriction pattern, consisting of :
- diminished lung volumes
- preserved flow rates
- low diffusion capacity
Pathology
The pathogenesis of pulmonary involvement relates to separate mechanisms:
- direct involvement
- scleroderma-related interstitial lung disease (SSc-ILD)
- usual interstitial pneumonia (UIP) pattern: histologically indistinguishable from rheumatoid lung and idiopathic pulmonary fibrosis (IPF)
- an NSIP type can also occur
- scleroderma-related pulmonary arterial hypertension (SSc-PAH)
- pathogenesis is unclear but may be due to vascular endothelial injury with subsequent apoptosis, inflammation and dysregulated angiogenesis leading to arterial obliteration and narrowing from fibrosis
- scleroderma-related interstitial lung disease (SSc-ILD)
- indirect involvement
- secondary lung injury due to aspiration pneumonitis secondary to esophageal involvement: see gastrointestinal manifestations of scleroderma
The two pathologies may co-exist. The remainder of the article discusses the former. Please refer to aspiration pneumonitis for discussion of that entity.
Radiographic features
Plain radiograph
Chest radiographs are insensitive to early changes and may appear normal despite respiratory function test abnormalities. Eventually, changes of pulmonary fibrosis become evident. Additional features include :
- dilated esophagus
- eggshell calcification of mediastinal nodes
- pleural effusions are uncommon
- enlargement of the cardiac silhouette and pulmonary arteries due to scleroderma induced pulmonary vascular disease may also be evident.
CT
On HRCT, scleroderma may appear in either a usual interstitial pneumonitis (UIP) or non-specific interstitial pneumonitis (NSIP) pattern (the latter is considered more common). Interstitial lung changes in scleroderma are less extensive and less coarse than those with idiopathic pulmonary fibrosis (IPF) with most patients only show a limited portion of lung involvement (less than 10% in half of cases) .
- early stages may show ground glass changes
- later stages may show honeycombing and evidence of lung volume loss
- lung bases and sub-pleural regions typically involved
- cysts may be present measuring 1-5 cm in diameter
- pleural effusions are usually not a feature
- CT may also show features of pulmonary hypertension and mediastinal lymphadenopathy
- bronchiectasis
- tends to be cylindrical in general
- maybe present in around 60% of patients according to one study
A dilated esophagus is not an uncommon finding.
Treatment and prognosis
Pulmonary involvement is incurable but some compounds may improve or halt progression. These include cyclophosphamide, glucocorticoids or N-acetylcysteine, although the data is inconclusive .
Complications include:
- pulmonary arterial hypertension is seen in up to 50% of patients and may develop without evidence of interstitial fibrosis
- higher incidence of lung cancer, particularly bronchoalveolar carcinoma
- rupture of pulmonary cysts resulting in a pneumothorax
The cause of death is often from aspiration pneumonia.
Differential diagnosis
On HRCT, the differential is essentially that of usual interstitial pneumonia and lower zone pulmonary fibrosis.
A helpful clue to the diagnosis on CT is the presence of a dilated esophagus.
Pleural effusions are distinctly uncommon in scleroderma and would favor the diagnosis of either rheumatoid lung or SLE .
See also
- musculoskeletal manifestations of scleroderma
- cardiac manifestations of scleroderma
- gastrointestinal manifestations of scleroderma
- hepatobiliary manifestations of scleroderma
- renal manifestations of scleroderma
Siehe auch:
- systemischer Lupus Erythematodes
- Systemische Sklerodermie
- gastrointestinale Manifestationen Sklerodermie
- rheumatoid lung
- muskuloskelettale Manifestationen bei Sklerodermie
und weiter:

 Assoziationen und Differentialdiagnosen zu pulmonary manifestations of scleroderma:
Assoziationen und Differentialdiagnosen zu pulmonary manifestations of scleroderma: