Hashimoto-Thyreoiditis









Hashimoto thyroiditis, also known as lymphocytic thyroiditis or chronic autoimmune thyroiditis, is a subtype of autoimmune thyroiditis. It is one of the most common thyroid disorders.
Epidemiology
Typically affects middle-aged females (30-50 year age group with an F:M ratio of 10-15:1).
Clinical presentation
Patients usually present with hypothyroidism +/- goiter. However, a very small proportion of cases (~5%) can present with hyperthyroidism (also known as Hashitoxicosis). There is often a gradual painless enlargement of the thyroid gland during the initial phase with atrophy and fibrosis later on in the course.
The Hashitoxicosis phase, if present, usually only lasts 1-2 months. Although rare cases last much longer .
Pathology
There is autoimmunity to the thyroid gland which bears both humoral- and cell-mediated features. This is followed by lymphocytic infiltration of the thyroid gland with lymphoid follicles replacing thyroid follicles. This may affect the thyroid gland in either a diffuse or focal manner. Cell populations include:
- lymphocytic aggregates
- transformed follicular cells (Askanazy/oxyphilic/Hurthle cells)
Later stages show superadded fibrosis.
Serological markers
- antithyroglobulin antibodies: found in ~70% of cases
- thyroid peroxidase antibodies (TPO): found in 90-95% of cases
Associations
- Turner syndrome
- primary thyroid lymphoma
- Hashimoto encephalopathy (rare)
- Down syndrome
- other autoimmune disorders
Radiographic features
Ultrasound
It is difficult to reliably sonographically differentiate Hashimoto thyroiditis from other thyroid pathology. Ultrasound features can be variable depending on the severity and phase of disease :
- diffusely enlarged thyroid gland with a heterogeneous echotexture is a common sonographic presentation (especially initial phase)
- the presence of hypoechoic micronodules (1-6 mm) with surrounding echogenic septations is also considered to have a relatively high positive predictive value ; this appearance may be described as pseudonodular or a giraffe pattern.
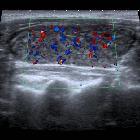
- color Doppler study usually shows normal or decreased flow, but occasionally there might be hypervascularity similar to a thyroid inferno
- the hypervascularity does not reflect thyrotoxicosis, indeed it appears to be more common in hypothyroid Hashimoto patients !
- prominent reactive cervical nodes may be present, especially in level VI, but they have normal morphologic features
- patients are at higher risk for papillary thyroid carcinoma, so a discrete nodule should be considered for biopsy
In some situations, large nodules may be present, which may be referred to as nodular Hashimoto thyroiditis .
Nuclear medicine
Radioactive iodine
- early stages: may show increased uptake
- late stages: single or multiple areas of reduced uptake (cold spots)
FDG PET
- diffuse high uptake throughout the thyroid is consistent with chronic thyroiditis (or a normal variant)
- superimposed focal high uptake should raise concern for a thyroid nodule including the possibility of carcinoma
History and etymology
It was first described in 1912 by Hakaru Hashimoto (1881-1934), a Japanese physician while working in Germany; in his original description, he called it 'struma lymphomatosa' .
Differential diagnosis
For ultrasound appearances consider:
Siehe auch:
- Morbus Basedow
- papilläres Schilddrüsenkarzinom
- Giraffe pattern
- Lymphom der Schilddrüse
- Hashimoto-Enzephalopathie
- Ord-Thyreoiditis
- Hashitoxikose
und weiter:

 Assoziationen und Differentialdiagnosen zu Hashimoto-Thyreoiditis:
Assoziationen und Differentialdiagnosen zu Hashimoto-Thyreoiditis:

