liver infarction

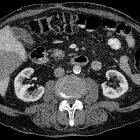
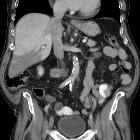




Hepatic infarction is an extremely rare situation because the liver has a dual blood supply from the hepatic artery and portal vein. Hepatic infarction can occur when there is both hepatic arterial and portal vein flow compromise but most cases are due to acute portal venous flow compromise .
Epidemiology
Most cases are seen after liver transplantation or hepatobiliary surgery. Non-transplant cases are mostly caused by :
- hepatic artery occlusion due to
- arteriosclerosis
- thrombosis or emboli
- hepatic artery aneurysm
- polyarteritis nodosa
- sickle cell disease
- infarction without hepatic artery occlusion is mainly caused by
- acute shock state/systemic hypotension
- trauma
- hypercoagulable state
- preeclampsia, eclampsia and postpartum HELLP syndrome
- complication of anesthesia
Clinical presentation
Clinically, these patients present with abdominal pain, nausea, vomiting and abnormal liver function tests . Most of the time, infarction is a peripherally located wedge-shaped area, however it can be centrally or round or oval shape .
Radiographic features
Ultrasound
- acute stage
- an ill-defined hypoechoic area with indistinct border
- gas within sterile infarcted zone can be seen
- chronic stage
- infarcted area becomes anechoic and cystic with distinct borders
Differentiation between gas within sterile infarcted area and abscess formation by imaging is impossible and fine needle aspiration is needed .
CT
Typically infarction presents as an ill-defined wedge-shaped area of hypoattenuation which is mostly peripheral without mass-effect on adjacent structures in post-contrast images .
MRI
On MRI imaging, regions of hepatic infarction appears as hypointense lesion on T1 imaging, with hyperintensity on T2 imaging .
Differential diagnosis
General imaging differential considerations include:
- focal hepatic steatosis: focal fatty infiltration also lacks mass effect, however vessels are seen crossing through the lesion
- hepatic abscess: typically shows mass effect on adjacent structures and ring-enhancement while hepatic infarction lacks mass-effect and any enhancement
- true hepatic masses: both mass effect and enhancement differentiate from hepatic infarction, and the clinical scenario is different
- emphysematous hepatitis: when gas is present, usually no mass effect
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Leberinfarkt:
Assoziationen und Differentialdiagnosen zu Leberinfarkt:
