periostales Osteosarkom
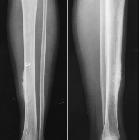



Periosteal osteosarcoma is a form of surface osteosarcoma.
Epidemiology
It is the second most common type of juxtacortical or surface osteosarcoma after parosteal osteosarcoma and accounts for 1.5% of all osteosarcoma cases. It affects a slightly older age group (10-20 years) cf. conventional osteosarcoma.
Pathology
Periosteal osteosarcoma arise from the inner germinative layer of periosteum. Cytologic grade of this tumor is higher than parosteal osteosarcoma and lower than conventional osteosarcomas, so it is considered as an intermediate grade osteosarcoma (grade 2). It predominantly contains chondroid matrix.
Location
- lesions tend to be diaphyseal
- femur and tibia most common, especially medial distal femur
- arises from cortex, being attached to underlying cortex at origin; intramedullary extension is rare
Radiographic features
Typically seen as a broad-based surface soft-tissue mass causing extrinsic erosion of thickened underlying diaphyseal cortex and perpendicular periosteal reaction extending into the soft-tissue component:
- predominantly chondroid matrix results in a lesion that is low in attenuation on CT images and hyperintense on T2 weighted MR images and tends to “wrap around” the circumference of the bone
- a periosteal reaction common, as sunburst pattern (radiating from bone surface) or a Codman triangle
MRI
- typically hypointense on both T1 and T2 sequences: may see bony spicules radiating from surface lesion (sunburst pattern)
- it may appear hyperintense on T2 sequence which represents its chondroid matrix.
- reactive marrow changes are commonly seen at MR imaging, but true marrow invasion is rare
- it is difficult to differentiate periosteal osteosarcoma from the conventional high grade osteosarcoma at imaging, however conventional osteosarcomas involve entire circumference of cortex and show intramedullary extension.
Treatment and prognosis
A periosteal osteosarcoma is of intermediate grade with prognosis being better than conventional osteosarcoma, but not as good as parosteal osteosarcoma (which is usually low grade).
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu periostales Osteosarkom:
Assoziationen und Differentialdiagnosen zu periostales Osteosarkom: