pleuroparenchymal fibroelastosis
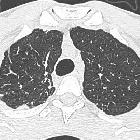


















Pleuroparenchymal fibroelastosis (PPFE) is a recently described rare, benign entity. About half of cases are felt to be idiopathic, with the other half secondary to underlying diseases or conditions (e.g. transplantation). Idiopathic cases belong to the group of idiopathic interstitial pneumonias.
Epidemiology
Pleuroparenchymal fibroelastosis is considered a rare disorder; however, it is very likely both under-recognized and misdiagnosed . Median age at presentation in reported cases approximates the 5 decade of life, with age distribution likely bimodal :
- early peak in the 3decade
- late peak in the 6decade
No gender predilection has been reported, and patients are most often non-smokers .
Clinical presentation
Most often significant chronic respiratory symptoms, which may include:
- non-productive cough
- dyspnea, either on exertion or in a worsening course
- angina
- frequent airway infections
Signs may include:
- pneumothorax
- positive autoimmune titers
- reduced lung function of a mixed (obstructive and restrictive) pattern (reduced forced expiratory in 1second (FEV1), reduced forced vital capacity (FVC), reduced diffusing capacity for carbon monoxide (DLCO))
Pathology
The pathophysiology is unknown. Pleuroparenchymal fibroelastosis is characterized by predominantly upper lobe pleural and subjacent parenchymal fibrosis (the latter being intra-alveolar with accompanying elastosis of the alveolar walls).
Etiology
The etiology remains unknown. Familial cases have been reported, especially in young women .
Roughly half of cases occur as a sequela of lung transplantation or bone marrow transplantation . About one-tenth might even be drug-induced by chemotherapy .
Histology
Typical features include the abundance of short, curled, and randomly oriented elastic fibers, resulting in elastic fibrosis of the visceral pleura. These may be identifiable on standard hematoxylin and eosin (H&E) stains, however elastic fiber stains (e.g. Elastica van Gieson (EVG)) may be useful in cases of doubt.
Radiographic features
Plain radiograph
Chest radiographs may be normal or present non-specific findings comprising:
- marked bilateral apical pleural thickening
- pneumothorax
CT
Optimally performed as high-resolution computed tomography (HRCT) of the lung, it may depict:
- marked bilateral apical pleural thickening
- apical caps
- pneumothorax
- architectural distortion, possibly leading to
- traction bronchiectasis
- upper lung volume loss
- peripheral consolidation
- reticular abnormalities, including
- thickening of interlobular septa
- honeycombing
- lymphadenopathy: mediastinal and/or axillary
Other accompanying chest wall features include
- platythorax which often denoted by the presence of a deep suprasternal notch and/or posterior retraction of the trachea.
Nuclear medicine
Hitherto one case has been described, presenting as a hypermetabolic pulmonary nodule on 18F-FDG-PET with associated hypermetabolic axillary lymphadenopathy .
Treatment and prognosis
Pleuroparenchymal fibroelastosis usually shows a progressive clinical course and carries a poor prognosis. There is currently no specific therapy. Medical options with steroids, cyclophosphamide, azathioprine, N-acetylcysteine, azithromycin, sulfamethoxazole and trimethoprim may all be tried. In progressive cases, lung transplantation may be required.
Complications
Postprocedural pneumothorax and/or bronchopleural fistula are often seen and may even raise clinical suspicion of this underlying entity .
History and etymology
It is thought to have been first described as idiopathic pulmonary upper lobe fibrosis in 1992 in Japanese literature by Aminati et al and thought to have been first described in an English paper by S K Frankel et al. in 2004 .
Differential diagnosis
For the relatively rare combination of both pleural and interstitial fibrosis may include :
- connective tissue diseases
- asbestosis
- sarcoidosis (advanced fibrosing type)
- radiation-induced lung disease: appropriate patient history
- drug-induced lung disease: correlate to patient history
- restrictive type of chronic lung allograft dysfunction (rCLAD): history of lung transplant
Siehe auch:
- medikamenteninduzierte Pneumonitis
- Hilusraffung
- Idiopathische interstitielle Pneumonie
- strahleninduzierte Lungenerkrankung
und weiter:

 Assoziationen und Differentialdiagnosen zu pleuroparenchymale Fibroelastose:
Assoziationen und Differentialdiagnosen zu pleuroparenchymale Fibroelastose:



