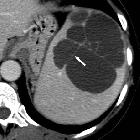
splenic pseudocyst








Splenic pseudocysts, also referred as secondary splenic cysts, are acquired cystic lesions not delineated by a true epithelial wall. They represent the majority of the splenic cystic lesions, corresponding to approximately 80% of them (c.f. splenic epithelial cysts). The main causes are:
- splenic trauma
- splenic infarction
- locoregional inflammation: e.g. intrasplenic pancreatic pseudocyst
Epidemiology
They are thought to account for 80% of benign non-parasitic cysts of the spleen .
Clinical presentation
Splenic pseudocysts, similarly to the splenic epithelial cysts, are mostly asymptomatic, with symptoms presenting only when they are big enough to cause some significant local mass effect .
Pathology
They are acquired lesions and, regardless if due to trauma or infarction, represent the end stage of splenic injury resultant liquefactive necrosis and cystic changes. Microscopically, there is no lining epithelium .
Radiographic features
Ultrasound
Usually present as well defined cystic lesions with heterogeneous content due to the presence of echoes (e.g. hematic debris).
CT
Typically shows a hypoattenuating (water-attenuated) relatively well-defined intrasplenic lesion. The margins are thin and have a sharp demarcation to the splenic parenchyma. Calcification may be present in the fibrous wall. There is no rim or internal enhancement.
MRI
Well-defined cystic lesions with an internal fluid signal intensity that may vary from completely homogeneous to heterogeneous, depending on the presence of hemorrhagic or proteinaceous content:
- T1: variable
- T2: very high signal intensity
Treatment and prognosis
Small and asymptomatic cysts do not require treatment or followup. Symptomatic cysts may be managed surgically or percutaneously drained .
Complications
Complications are rare and include hemorrhage, rupture and infection .
Differential diagnosis
A number of splenic lesions may appear cystic, depending on the modality:
- primary splenic cysts (~20% of all splenic cysts)
- infection
- splenic hydatid cyst
- splenic bacterial abscess
- other congenital cystic lesions (tend to be unilocular in a majority of cases)
- cystic splenic metastases
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Pseudozyste der Milz:
Assoziationen und Differentialdiagnosen zu Pseudozyste der Milz: