differential diagnosis of tracheomalacia

Mounier-Kuhn
syndrome. Chest X-ray PA and lateral view showed tracheomegaly (arrows)

Mounier-Kuhn
syndrome. Contrast-enhanced transverse CT scan obtained at different levels with mediastinal/lung window setting showed dilated trachea and small diverticula (yellow arrow) and a few cystic bronchiectasis in the right lower lobe (red arrow)

Mounier-Kuhn
syndrome. Coronal and sagittal reformatted images with lung window setting: tracheomegaly with irregularity of the tracheal wall, multiple sacculations and with cystic bronchiectasis (arrow) in the right lower lobe

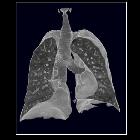
Mounier-Kuhn
syndrome. The post-processed thick minimal intensity images (MinIP) were particularly useful in demonstrating dilatation and irregularity of tracheobronchial tree with absence of the cavities at the lung periphery.

Tracheomalacia
(differential) • Acquired tracheobronchomalacia - Ganzer Fall bei Radiopaedia

Tracheomalacia
(differential) • Mounier-Kuhn disease - Ganzer Fall bei Radiopaedia
A dilated trachea has numerous causes, and in almost all cases represents tracheomalacia (increased size and increased compliance).
As is almost always the case, various diameters have been used. Typical figures include >26 mm in men, >23 mm in women or >3 cm for both genders.
Although many of the underlying conditions are congenital, actual dilatation of the trachea and symptomatic presentation are only later in adulthood. Thus the term congenital in the list below refers to the underlying cause, rather than presence of tracheomegaly at birth.
Congenital
- cystic fibrosis
- Mounier-Kuhn syndrome (tracheobronchomegaly)
- idiopathic or associated with:
- Ehlers-Danlos syndrome (in adults)
- cutis laxa (in children)
- Marfan syndrome
- Kenny-Caffey syndrome
- Cornelia-de Lange syndrome
- Bruton-type agammaglobulinemia
- ataxia telangiectasia
Acquired
Acquired tracheomalacia is a common finding, seen in approximately 10% of CT and up to 23% of autopsy and bronchoscopy series .
Common
- normal aging
- prolonged intubation, especially in those with a tracheostomy
- chronic obstructive pulmonary disease (chronic bronchitis / emphysema)
- diffuse pulmonary fibrosis, especially secondary to radiation
Uncommon
- relapsing polychondritis
- playing wind instruments
- inhalation of noxious fumes
- ataxia-telangiectasia
- ankylosing spondylitis
- light-chain deposition disease
Siehe auch:
- Morbus Bechterew
- Ehlers-Danlos syndrome
- Marfan-Syndrom
- zystische Fibrose
- Tracheomalazie
- Cornelia-de-Lange-Syndrom
- Rezidivierende Polychondritis
- angeborene Tracheobronchomegalie
- Emphysem
- ataxia-telangiectasia
- diffuse pulmonary fibrosis
und weiter:

 Assoziationen und Differentialdiagnosen zu Differenzialdiagnosen bei Tracheomalazie:
Assoziationen und Differentialdiagnosen zu Differenzialdiagnosen bei Tracheomalazie:







