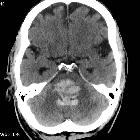
cerebellar hemorrhage













Cerebellar hemorrhage is a form of intracranial hemorrhage and is most frequently seen in the setting of poorly controlled hypertension, although this can of course also be secondary to an underlying lesion (e.g. tumor or vascular malformation) or due to supratentorial surgery (see remote cerebellar hemorrhage).
This article concerns itself with primary cerebellar hemorrhages.
Epidemiology
The demographics of affected patients reflect those of patients with long term poorly controlled hypertension, and as such patients are usually elderly.
Cerebellar hemorrhages only account for approximately 10% of all intracerebral hemorrhages .
Clinical presentation
Clinical presentation depends on the size and speed of enlargement of the hemorrhage. Unlike pontine hemorrhages which are usually obvious to both the clinician and the patient, cerebellar hemorrhages, if small enough, can present relatively subtly. Cerebellar signs (e.g. ataxia, nystagmus) . Larger bleeds can impair consciousness and obstruct the fourth ventricle resulting in obstructive hydrocephalus.
Radiographic features
CT
As with other hemorrhagic strokes, CT is usually the first, and often the only imaging investigation obtained.
As with other acute hemorrhages, cerebellar hemorrhages appear as regions of hyperdensity within the cerebellar hemispheres. Extension into the fourth ventricle or subarachnoid space is relatively common.
If there is no extension into the ventricular system, the volume of the hemorrhage can be estimated using ABC/2 and related formulas, which may have neurosurgical and prognostic implications.
Treatment and prognosis
Unlike pontine hemorrhages, cerebellar hemorrhages carry a relatively good prognosis if timely evacuation and control of hydrocephalus can be obtained.
Prompt diagnosis and neurosurgical referral are therefore key. Typically if a hemorrhage causes brainstem compression or is greater than 3 cm in diameter (20-30 mL) then evacuation is beneficial .
Siehe auch:
- Intrazerebrale Blutung
- Hydrocephalus
- Intrakranielle Blutung
- Ponsblutung
- Verschlusshydrocephalus
- vierter Ventrikel
- Hirnblutung mit Ventrikeleinbruch
- hyperdense zerebrale Metastasen
- Remote cerebelläre Blutung
- pontine haemorrhages
und weiter:

 Assoziationen und Differentialdiagnosen zu Kleinhirnblutung:
Assoziationen und Differentialdiagnosen zu Kleinhirnblutung: