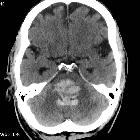
intracranial hemorrhage







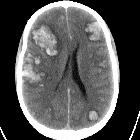




Intracranial hemorrhage (ICH) is a collective term encompassing many different conditions characterized by the extravascular accumulation of blood within different intracranial spaces. A simple categorization is based on location:
- intra-axial hemorrhage
- extra-axial hemorrhage
Alternatively, intracranial hemorrhage can be thought of in terms of the underlying cause, although in most cases the same etiology can result in multiple different patterns of hemorrhage.
- trauma
- vascular malformation(s)
- tumor related hemorrhage
- hypertension: hypertensive hemorrhage
- cerebral amyloid angiopathy (CAA)
- cerebral venous thrombosis
Radiographic features
CT
CT scan is almost always the first imaging modality used to assess patients with suspected intracranial hemorrhage. Fortunately, acute blood is markedly hyperdense compared to brain parenchyma, and as such usually poses little difficulty in diagnosis (provided the amount of blood is large enough, and the scan is performed early).
CT angiography (CTA) is increasingly used to assess for a vascular underlying cause, particularly in cases of subarachnoid hemorrhage, or intraparenchymal hemorrhage where something in the presentation, demographics of the patient, or location/appearance of bleed make a primary hemorrhage less likely.
Similarly, CT venogram (CTV) can be used to reliably assess for patency of the dural venous sinuses.
MRI
MRI is typically requested when an underlying abnormality is being sought, particularly when an underlying tumor is suspected. MRI of hemorrhage can pose some challenges in that the appearance of blood changes depending on the sequence and the time since the hemorrhage and the size and location of the bleed.
Angiography
Cerebral angiography is usually performed when a vascular abnormality is suspected and the CT/MR angiogram is either normal (and index of suspicion is high) or equivocal, or in cases where further delineation or treatment of an identified abnormality is required.
Siehe auch:
- Unterscheidung epidurales Hämatom subdurales Hämatom
- Intrazerebrale Blutung
- Zerebrale Amyloidangiopathie
- Arteriovenöse Malformation
- Subarachnoidalblutung
- subdurales Hämatom
- Altersbestimmung Blutung MRT
- intraventrikuläre Blutung
- durale AV-Fistel
- epidurales Hämatom
- Ponsblutung
- Einblutung in die Basalganglien
- Lobärblutung
- Kleinhirnblutung
- Duret Blutungen
- zerebrale Venenthrombose
- sakkuläre zerebrale Aneurysmata
- zerebrale Kontusionsblutung
- intracranial hemorrhage evaluation with mri
und weiter:
- Einklemmung
- lacunar stroke syndrome
- Coup-Contre-coup-Mechanismus
- Hämophilie
- Thrombozytopenie-Radiusaplasie-Syndrom
- intracranial haemorrhage with fluid-fluid level
- fetal intracranial haemorrhage
- Einteilung Hirnblutung
- Hämosiderinablagerungen nach intrazerebraler Blutung
- moya moya with haemorrhage
- primäre intraventrikuläre Blutung
- Blutung bei intrakranieller AV-Malformation
- Kontroll CT nach Blutung
- swirl sign of intracranial haemorrhage
- Hirnherniation
- Hämorrhagien nach Schlangenbiss

 Assoziationen und Differentialdiagnosen zu Intrakranielle Blutung:
Assoziationen und Differentialdiagnosen zu Intrakranielle Blutung: