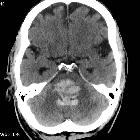
Hypertensive intracerebral hemorrhage

Hypertensive
intracerebral hemorrhage • Hypertensive basal ganglial bleed - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Hypertensive hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Cerebellar hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Hypertensive intracerebral hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Thalamic hematoma and intraventricular hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Cerebellar hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Combined traumatic and hypertensive hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Pontine and basal ganglia hypertensive hemorrhages - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Hypertensive intracerebral hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Hypertensive intracerebral hemorrhage - Ganzer Fall bei Radiopaedia

Hypertensive
intracerebral hemorrhage • Hypertensive intracerebral hemorrhage with intraventricular extension - Ganzer Fall bei Radiopaedia

Charcot-Bouchard
aneurysm • Hypertensive basal ganglial bleed - Ganzer Fall bei Radiopaedia
Hypertensive intracerebral hemorrhages are common. In fact, hypertension is the most common cause of intracerebral hemorrhages. They can be conveniently divided according to their typical locations which include, in order of frequency:
- basal ganglia hemorrhage (especially the putamen)
- thalamic hemorrhage
- pontine hemorrhage
- cerebellar hemorrhage
Clinical presentation
Patients will present depending on the region and size of the hemorrhage:
- basal ganglia hemorrhage usually presents with ipsilateral deviation of the eyes due to descending capsular pathways from the frontal eye field
- thalamic hemorrhage often presents with downward deviation of eyes and lack of pupillary response to light
- pontine hemorrhage usually causes coma due to disruption of the reticular activating system (unless small) and quadriparesis due to disruption of the corticospinal tract
Pathology
Long-standing poorly controlled hypertension leads to a variety of pathological changes in the vessels.
- microaneurysms of perforating arteries (Charcot-Bouchard aneurysms)
- small (0.3-0.9 mm) diameter
- occur on small (0.1-0.3 mm) diameter arteries
- distribution which matches the incidence of hypertensive hemorrhages
- 80% lenticulostriate
- 10% pons
- 10% cerebellum
- found in hypertensive patients
- may thrombose, leak (see cerebral microhemorrhages) or rupture
- accelerated atherosclerosis: affects larger vessels
- hyaline arteriosclerosis
- hyperplastic arteriosclerosis: seen in very elevated and protracted cases
Treatment and Prognosis
Hemorrhage causes displacement of brain tissue, but once resorbed, the patient recovers with fewer deficits compared to similar-sized infarcts. Characteristics of hypertensive hemorrhages that lead to poorer prognosis include :
- bleed in the posterior fossa
- large amount of mass effect
- extension into the ventricular system
Video
Siehe auch:
- Intrazerebrale Blutung
- Ponsblutung
- zerebrale Mikroblutungen
- Einblutung in die Basalganglien
- Kleinhirnblutung
- Arterielle Hypertonie
- Atherosklerose
- zerebrale Mikroangiopathie bei Hypertonus
und weiter:

 Assoziationen und Differentialdiagnosen zu hypertensive Hirnblutung:
Assoziationen und Differentialdiagnosen zu hypertensive Hirnblutung: