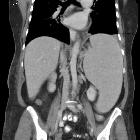
congenital cytomegalovirus infection










Congenital cytomegalovirus infections result from intrauterine fetal infection by cytomegalovirus (CMV).
Epidemiology
Cytomegalovirus is the most common cause of intrauterine infection and the most common cause of congenital infective and brain damage, occurring in 0.2-2.4% of live births.
Antibodies to cytomegalovirus are seen in 30-60% of pregnant women, but only 2.5% have a primary infection during pregnancy, and this can result in fetal infection in ~30% of cases.
Clinical presentation
The vast majority (90%) of infected babies are asymptomatic at birth, but some may go on to develop symptoms after 6-9 months. Some countries now keep spots of neonatal blood on special filter paper (Guthrie cards) for cytomegalovirus DNA testing at a later date if needed.
Possible signs and symptoms include:
- jaundice/hepatomegaly/splenomegaly
- microcephaly
- sensorineural deafness
- chorioretinitis
- petechiae
- blueberry muffin rash
- intellectual disability
- seizures
The degree of neurological impairment is variable, from mild learning and behavioral problems to intellectual disability and physical handicaps.
Pathology
Cytomegalovirus (CMV) is a DNA virus in the herpes virus family which has the propensity to cause intrauterine infections and is part of the group referred to as TORCH infections.
Radiographic features
Ultrasound
Brain
- fetal intracranial calcification: mainly periventricular calcification (hyperechogenic foci), considered one of the commonest of features
- fetal hydrocephalus
- heterogeneous appearing parenchyma
- microcephaly
- intraventricular adhesions
Other
- fetal intrahepatic calcification
- fetal hepatomegaly
- evidence of intrauterine growth restriction (IUGR)
- echogenic bowel
These findings are associated with poor outcome, allowing mothers to consider termination of the pregnancy if identified early enough.
CT
CT brain
When performed postnatally, non-contrast CT demonstrates variable features, including:
- intracranial calcifications: particularly thick and chunky in germinal matrix and periventricular regions with faint and punctate basal ganglia calcifications
- white matter low density regions
- ventriculomegaly/cerebral atrophy/destructive encephalopathy
- neuronal migration disorders
MRI
MRI brain
Features seen on MRI include:
- microcephaly
- white matter lesions: periventricular subependymal cysts representing focal areas of necrosis. They are predominantly parietal or posterior white matter involvement with spared rim in immediately periventricular and subcortical white matter.
- ventriculomegaly and subarachnoid space enlargement
- delayed myelination
- periventricular and temporal pole cysts
- migrational abnormalities: lissencephaly, pachygyria, cortical dysplasia, polymicrogyria and schizencephaly
Complications
- cytomegalovirus encephalitis
- development of hydrops fetalis: in an in utero situation if severe
Siehe auch:
- fetal intracranial calcification
- Splenomegalie
- Hydrops fetalis
- Mikrozephalie
- fetal hepatomegaly
- Hepatomegalie
- Intrauterine Wachstumsretardierung
- Virusenzephalitis
- in utero infection
- Zytomegalievirus Enzephalitis
- fetal intra-hepatic calcification
- TORCH infections
- pädiatrische zerebrale Infektionen
- kongenitaler Hydrozephalus
- echogenic bowel
und weiter:

 Assoziationen und Differentialdiagnosen zu connatale Zytomegalie:
Assoziationen und Differentialdiagnosen zu connatale Zytomegalie: