septic arthritis











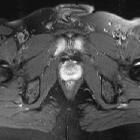


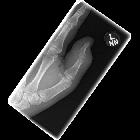








Septic arthritis is a destructive arthropathy caused by an intra-articular infection that is usually related to severe symptoms such as pain and decreased range of motion. This condition requires prompt treatment aiming to avoid permanent damage to joint, which may result in chronic deformity or mechanical arthritis and even death .
Clinical presentation
The diagnosis of joint sepsis is often considered straightforward. Patients often present with a painful joint, fever and purulent synovial fluid.
Pathology
Risk factors for septic arthritis include bacteremia, advanced age, an immunocompromised state, rheumatoid arthritis, intra-articular injections, and prosthetic joints.
In the absence of trauma or recent instrumentation of the joint, septic arthritis is usually secondary to haematogenous seeding. Staphylococcus aureus is the most commonly isolated agent .
Location
Large joints with abundant blood supply to the metaphyses are most prone to bacterial infection, with the most commonly affected joints theoretically being the shoulder, hip, and knee.
In intravenous drug abusers, the sternoclavicular and sacroiliac joints are more frequently affected.
Radiographic features
Imaging generally plays an adjunct role to arthrocentesis in the diagnosis of joint sepsis. If synovial fluid cannot be retrieved, however, radiologic studies become of the utmost importance.
Plain radiograph
- may be normal in the very early stage of the disease
- joint effusion may be seen
- juxta-articular osteoporosis due to hyperemia
- narrowing of the joint space due to cartilage destruction in the acute phase
- destruction of the subchondral bone on both sides of a joint
- if left untreated, reactive juxta-articular sclerosis and, in severe cases, ankylosis will develop
Ultrasound
- useful in superficial joints and in children
- shows joint effusion
- echogenic debris may be present
- color Doppler may show increased peri-synovial vascularity
- can be used to guide the joint aspiration
CT
- CT features of septic arthritis are similar to those spotted on radiographs
- a fat-fluid level can be a specific sign in the absence of trauma
MRI
- sensitive and more specific for early cartilaginous damage
- T1: low signal within the subchondral bone
- T2: perisynovial edema
- C+ (Gd): synovial enhancement
Treatment and prognosis
The treatment principle for septic arthritis is prompt drainage of purulent fluid and appropriate antibiotics .
If the patient is hemodynamically stable then attempts should be made to obtain a sample of joint fluid for microscopy and culture prior to starting treatment with antibiotics. This will allow focused treatment of the infection .
With smaller joints needle drainage or aspiration to decompress the joint followed by antibiotics may be adequate. For larger joints or persistent infection, surgical debridement and washout will be required .
If unrecognised and left untreated, septic arthritis can result in irreversible joint damage within 48 hours of the onset of infection due to the proteolytic enzymes of the white blood cells that flood the infected synovial space. Osteonecrosis is also an important sequela of septic arthritis due to effusion and increase in intra-articular pressure compromises blood circulation.
Conversely, approximately 90% of patients with septic arthritis will recover with appropriate antibiotic treatment. Therefore, timely diagnosis and treatment are critical.
See also
Siehe auch:
- Osteomyelitis
- Rheumatoide Arthritis
- Gelenkerguss
- infektiöse Myositis
- Zellulitis
- infizierte Hüftprothesen
- Arthritis urica
- spinal discitis-osteomyelitis
und weiter:
- Girdlestone-Operation
- Epiphyseolysis capitis femoris
- Sakroiliitis
- Milwaukee-Schulter
- differential diagnosis for metatarsal region pain
- transiente Osteoporose der Hüfte
- musculoskeletal manifestations of AIDS
- septicaemia
- Aseptische Nekrose des Metakarpale-Köpfchens
- Gelenkerguss Kiefergelenk
- Knochenmarködem-Syndrom (KMÖS)
- Arthritis der Schulter
- Schulterempyem
- superficial cellulitis
- Hunka classification
- Hüftgelenkserguss
- septic arthritis in ankylosing spondylitis
- septic arthritis of neonatal knee

 Assoziationen und Differentialdiagnosen zu Septische Arthritis:
Assoziationen und Differentialdiagnosen zu Septische Arthritis:




