Rheumatoide Arthritis








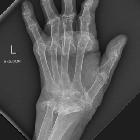

















Rheumatoid arthritis (RA) is a chronic autoimmune multisystemic inflammatory disease that affects many organs but predominantly attacks the synovial tissues and joints.
Epidemiology
The overall prevalence is 0.5-1% and the disease is 2-3 times more common in women .
Onset is generally in adulthood, peaking in the 4 and 5 decades. The pediatric condition, juvenile rheumatoid arthritis, is discussed separately.
Risk factors
- smoking (seropositive RA)
- obesity
- low socioeconomic status
Associations
- Felty syndrome: rheumatoid arthritis, splenomegaly, and neutropenia
- Caplan syndrome : rheumatoid arthritis and pneumoconiosis
Clinical presentation
Onset may be insidious or abrupt. Early features commonly include tiredness, malaise, and generalized aches. Arthritis symptoms typically first develop in the hands and wrists in a symmetric, proximal distribution. Feet and large joints may also be involved.
Pathology
Etiology is unknown but is probably multifactorial. It is generally considered that a genetic predisposition (HLA-DR B1 which is the most common allele of HLA-DR4 involved in rheumatoid arthritis) and an environmental trigger (Epstein-Barr virus postulated as a possible antigen, but not proven) lead to an autoimmune response that is directed against synovial structures and other organs.
Activation and accumulation of T CD4 cells in the synovium start a cascade of inflammatory responses which result in:
- activation of the macrophages and synovial cells and production of cytokines such as IL4 and TNF, which in turn cause proliferation of the synovial cells and increase the production of destructive enzymes such as elastase and collagenase by macrophages
- activating B cell lymphocytes to produce various antibodies including rheumatoid factor (RF-IgM antibodies against Fc portion of the IgG) which makes immune complexes that deposit in different tissues and contribute to further injury
- directly activate endothelial cells via increased production of VCAM1, which increases the adhesion and accumulation of inflammatory cells
- producing RANKL which in turn activate osteoclasts causing subchondral bone destruction
The inflammatory response leads to pannus formation. Pannus is an edematous thickened hyperplastic synovium infiltrated by lymphocytes T and B, plasmocytes, macrophages, and osteoclasts. Pannus will gradually erode bare areas initially, followed by the articular cartilage. It causes fibrous ankylosis which eventually ossifies .
Diagnostic criteria
Diagnosis is based on a combination of clinical, radiographic, and serological criteria. The 2010 ACR - EULAR classification criteria for Rheumatoid Arthritis has a maximal score of 10 and requires a score of >6 for a diagnosis of rheumatoid arthritis to be made:
- joint involvement
- 0: 1 large joint
- 1: 2-10 large joints
- 2: 1-3 small joints (with or without the involvement of large joints)
- 3: 4-10 small joints (with or without the involvement of large joints)
- 5: >10 joints (at least 1 small joint)
- serology
- 0: negative RF and negative anti-CCP
- 2: low-positive RF or low-positive anti-CCP
- 3: high-positive RF or high-positive anti-CCP
- acute phase reactants
- duration of symptoms
- 0: <6 weeks
- 1: >6 weeks
Non-musculoskeletal features of rheumatoid arthritis tend to occur late in the disease and include:
- pulmonary involvement
- disease may involve the interstitium, airway, and/or pleura
- cardiovascular disease
- accelerated coronary artery and cerebrovascular atherosclerosis contributing significantly to the excess mortality of RA
- pericarditis
- vasculitis: occurs more commonly with severe erosive disease, rheumatoid nodules, high RF titers
- cutaneous involvement
- rheumatoid nodules are usually seen in pressure areas: elbows, occiput, lumbosacral
- occurs in RF-positive patients
- ocular involvement
Markers
There are several serological markers for rheumatoid arthritis:
- rheumatoid factor (RF): is an IgM antibody against FC portion of the IgG antibodies, and is a traditional marker but is non-specific; associated with several autoimmune and chronic infectious diseases
- anti-cyclic citrullinated peptide (anti-CCP)/anti-citrullinated plasma antibody (ACPA): it is more than 80% sensitive and more than 95% specific
- elevated CRP or ESR
Radiographic features
Musculoskeletal
Musculoskeletal manifestations are the earliest and dominant features of rheumatoid arthritis.
For further details, please refer to musculoskeletal manifestations of rheumatoid arthritis.
Respiratory
Pulmonary rheumatoid disease may involve the airway, interstitium, and/or pleura; a full description is available in respiratory manifestations of rheumatoid arthritis.
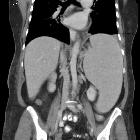
Abdominal
Splenomegaly may be seen as part of Felty syndrome, usually in long-standing rheumatoid arthritis.
Treatment and prognosis
Treatment of rheumatoid arthritis is aimed at improving the symptoms and slowing disease progression. Therapy is with a combination of corticosteroids, non-steroidal anti-inflammatory drugs (NSAIDs), disease-modifying anti-rheumatic drugs (DMARDs), and TNF antagonists (e.g. etanercept) The anti-TNF treatments and variants, which suppress the immune system, are known collectively as biological therapies.
The disease carries a significant burden of disability. There is also a reduction in life expectancy, with excess mortality usually related to its non-articular manifestations .
History and etymology
Rheumatoid arthritis was a term first coined by British physician Sir Alfred Baring Garrod (1819-1907) in 1859 .
Differential diagnosis
- psoriatic arthritis
- distal distribution, new bone formation, enthesis
- erosive osteoarthritis
- distal distribution, central erosions, and 'gull wing' formation
- systemic lupus erythematosus
- non-erosive MCPJ subluxation
- robust rheumatoid arthritis
Siehe auch:
- Splenomegalie
- Vaskulitis
- Aortitis
- Perikarditis
- pulmonale Manifestationen rheumatoide Arthritis
- Caplan-Syndrom
- rheumatoide Arthritis von Hand und Handgelenk
- Juvenile idiopathische Arthritis
- Uveitis
- Felty syndrome
- tuberculous arthritis
- Rheumatoide Arthritis Halswirbelsäule
- Synovialitis
- episcleritis
- palindromer Rheumatismus
- Rheumatoide Arthritis Ellenbogen
- chronic pyogenic arthritis
- muskuloskelettale Manifestationen rheumatoide Arthritis
- keratoconjunctivitis sicca
- general discussion of rheumatoid arthritis
- rheumatoid arthritis spine
und weiter:
- avascular necrosis causes (mnemonic)
- dural enhancement
- Ankylose
- Kryptogene organisierende Pneumonie (COP)
- Basiläre Impression
- Bronchiolitis obliterans
- Protrusio acetabuli
- inflammatorischer Pseudotumor der Orbita
- animal and animal produce inspired signs
- Patellarsehnenruptur
- Fibrothorax
- Sakroiliitis
- subchondrale Zysten
- Kardiomegalie
- Amyloidose
- Psoriasisarthritis
- Tendovaginitis stenosans de Quervain
- tree in bud-Muster
- Septische Arthritis
- lymphozytisch interstitielle Pneumonie
- Achillessehnenruptur
- Aneurysma Aorta ascendens
- Interstitielle Lungenerkrankung
- Auftreibung Metaphysen
- erosive Arthrose
- Tendovaginitis
- oberflächliche Weichteilläsionen der Extremitäten
- Jaccoud-Arthropathie
- bilaterale axilläre Lymphadenopathie
- conditions involving skin and bone
- fibrosierende Mediastinitis
- adult chest radiograph common exam pathology
- high riding shoulder
- Osteolyse der distalen Klavikula
- Boxerknöchel
- Pneumonitis
- basilar invagination (mnemonic)
- differential diagnosis for metatarsal region pain
- Weichteiltumoren der Extremitäten
- Knopflochdeformität
- Rheuma Differentialdiagnose
- Erlenmeyer flask deformity of the femur
- hypertrophe Pachymeningitis
- ACJ erosion
- temporomandibular joint inflammation
- Rheumatoide Arthritis des Dens axis
- anterior hip pain
- dens erosion
- vertebral body squaring
- distal clavicular erosion
- subkutane Rheumaknoten
- Aseptische Nekrose des Metakarpale-Köpfchens
- Mannerfelt-Zyste
- follikuläre Bronchiolitis
- differential diagnosis of calcific axillary lymphadenopathy
- a bakers cyst with rice body formation in a patient with rheumatoid arthritis.
- Gelenkerguss Kiefergelenk
- manubriosternale Ankylose
- Rheumazeichen
- Befallsmuster Arthritis
- Insuffizienzfrakturen des Beckens
- Schwanenhalsdeformität
- Rheumaknoten
- gold deposits in axillary lymph nodes
- rheumatoide Arthritis der Schulter
- Rheuma
- methotrexate-affected lungs in the case of rheumatoid arthritis
- Ulnardeviation
- Cushing-Syndrom
- Verdickungen der Achillessehne
- boutonierre deformity
- konventionelle Röntgendiagnostik bei der rheumatoiden Arthritis
- Hüftgelenkserguss
- Rheumatoide Arthritis Hüftgelenk
- Pannus Densspitze
- Pannus
- pulmonale hyaline Granulomatose
- Arthritis der Hand
- Dilatation der Aorta thoracica
- chronische Periaortitis

 Assoziationen und Differentialdiagnosen zu Rheumatoide Arthritis:
Assoziationen und Differentialdiagnosen zu Rheumatoide Arthritis: