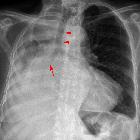
tension pneumothorax



























Tension pneumothoraces occur when intrapleural air accumulates progressively in such a way as to exert positive pressure on mediastinal and intrathoracic structures. It is a life-threatening occurrence requiring both rapid recognition and prompt treatment to avoid a cardiorespiratory arrest.
A non-tension pneumothorax is properly called a simple pneumothorax.
For a general discussion, refer to the pneumothorax article.
Clinical presentation
Presentation is variable and may initially have no symptoms. With time severe dyspnea, tachycardia and hypotension occur. Distended neck veins and tracheal deviation are also often present. Eventually, impaired venous return results in cardiac arrest and death. This can occur within minutes.
Clinical signs of a tension pneumothorax in the ventilated patient are comparably rapid, with arterial and mixed venous peripheral capillary oxygen saturation immediately decreasing .
Pathology
A tension pneumothorax occurs due to the progressive accumulation of intrapleural gas in thoracic cavity caused by a valve effect during inspiration/expiration. In this situation, the ipsilateral lung will, if normal, collapse completely (although a less than normally compliant lung may remain partially inflated). In either case, as the collection grows further, it exerts a positive mass effect on the mediastinum (compression of vessels and heart) and the opposite lung.
Radiographic features
A tension pneumothorax will have the same features as a simple pneumothorax with a number of additional features, helpful in identifying tension. These additional signs indicate hyperexpansion of the hemithorax:
- ipsilateral increased intercostal spaces
- contralateral shift of the mediastinum
- depression of the hemidiaphragm
In the rare instance of bilateral tension pneumothoraces there may be no cardiomediastinal shift .
Ultrasound
In addition to the sonographic features of pneumothorax, a RUSH exam (often performed in the setting of hemodynamic instability) the following features imply the presence of tension physiology ;
- fixed, dilated inferior vena cava
- visualized from a subcostal window, the IVC diameter and respirophasic variation can be used as a rough correlate of central venous pressure
- dilation (> 2.1 cm) and absence of variation with respiration imply a pathologically elevated CVP, consistent with obstructive shock
- hyperdynamic right heart with underfilling
- right ventricular function will be normal or supranormal, with systolic obliteration of the ventricular cavity
- in cardiac tamponade, another etiology in the differential for obstructive shock, right ventricular diastolic collapse will be observed
- the right ventricular diameter will be reduced as a result of the reduction in filling/preload
- right ventricular function will be normal or supranormal, with systolic obliteration of the ventricular cavity
Treatment and prognosis
Treatment of a tension pneumothorax is one of the classic medical emergencies where life can be saved or lost on the basis of recognition and subsequent rapid decompression. Numerous techniques exist, and the literature is replete with opinions, but in the first instance relieving the tension, even if not draining the pneumothorax, is life-saving. A needle thoracostomy (e.g. 14G intravenous cannula) can be inserted, typically in the 2 intercostal space in the midclavicular line, to gain valuable time, before a larger underwater drain can be inserted .
Differential diagnosis
- giant bullous emphysema: differentiated from tension pneumothorax by clinical stability, interstitial vascular markings projected with the bullae and lack of hemithorax re-expansion following the insertion of an intercostal catheter
- tension gastrothorax: differentiated by the poor definition of the left hemidiaphragm, lack of a gastric bubble, and potential air-fluid level
See also
Siehe auch:
und weiter:

 Assoziationen und Differentialdiagnosen zu Spannungspneumothorax:
Assoziationen und Differentialdiagnosen zu Spannungspneumothorax: