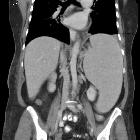
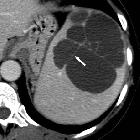
Raumforderungen der Milz

Hämangiom
der Milz mit typischem Irisblendenphänomen: Oben arteriell mit randständiger Kontrastmittelaufnahme, unten portalvenös aufgefüllt. (nicht histologisch bestätigt, aber typisch)

Littoralzellangiome
der Milz in der Magnetresonanztomografie: Links T2 und T1, rechts Kontrastmitteldynamik.

Hämangiom
der Milz in der Magnetresonanztomografie: Links T2 und T1, rechts Kontrastmitteldynamik mit Irisblendenphänomen.

Surgical
treatment of benign splenic lesions in pediatric patients: a case series of 30 cases from a single center. Imaging pictures (contrast CT) with corresponding pathology pictures (HE staining) of splenic focal lymphatic malformation, SANT, and splenic hamartoma. A, B Splenic focal lymphatic malformation (Case 30, black arrow shows focal endothelial papillary projections). C, D: SANT (Case 3, CT shows a typical “spoke-wheel” sign). E, F: Splenic hamartoma (Case 2, CT shows a heterogeneously enhanced hypodense mass)

Splenic
inflammatory (myofibroblastic) tumour: CT and MRI findings. Arterial-phase (b,c) images showed inhomogeneous, predominantly peripheral enhancement of the demarcated splenic mass (arrowheads).

Splenic
inflammatory (myofibroblastic) tumour: CT and MRI findings. Peripheral contrast enhancement progressed during the portal venous (d,e) phase. The ovoid splenic mass (arrowheads) appeared to be well-demarcated and measured approximately 4.5x6 cm.

Splenic
inflammatory (myofibroblastic) tumour: CT and MRI findings. Coronal (a), axial (b) and fat-suppressed (c) T2-weighted images confirmed well-demarcated ovoid lesion (arrowheads) at the upper splenic pole, with lower signal intensity peripherally compared to the spleen (*).

Sclerosing
angiomatoid nodular transformation of the spleen mimicking metastasis of melanoma: a case report and review of the literature. a B-mode ultrasound picture of the lesion. b, c, d Contrast-enhanced ultrasound image 19, 72, and 152 seconds after injection of 1 ml SonoVue®
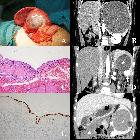
Surgical
treatment of benign splenic lesions in pediatric patients: a case series of 30 cases from a single center. Splenic CECs (“*” marks the cysts). A A recurrent cyst after unroofing (Case 21). B The cyst compressing left renal and renal artery (Case 26). C Stratified squamous epithelium (HE staining). D Simultaneous separate CEC and hemagioma (white arrow shows the enhanced hemangioma, Case 19). E Cytokeratin immunohistochemical staining labels the epithelium. F Simultaneous separate CEC and omentum mesothelial cyst (white triangle shows the omentum mesothelial cyst, Case 28)

Surgical
treatment of benign splenic lesions in pediatric patients: a case series of 30 cases from a single center. Splenic vascular malformations. A CT of splenic diffused lymphangiohemangiomatosis (white arrow shows the accessory spleen involved, Case 25). B Intraoperative picture of Case 25. C MRI of splenic diffused lymphangiomatosis (Case 20). D Intraoperative picture of Case 20. E HE staining of Case 25 shows lymphatic malformation space filled with eosinophilic amorphous proteinaceous fluid (black arrow) and capillary malformation space filled with blood (hollow arrow). F D2-40 immunohistochemical staining of Case 20 labels lymphatic endothelium

Sclerosing
angiomatoid nodular transformation of the spleen mimicking metastasis of melanoma: a case report and review of the literature. a Computed tomography scan of the abdomen showing two hypodense lesions of the spleen. b, c Magnetic resonance imaging of the abdomen showing the two lesions in T1 and T2 mode, respectively
Raumforderungen der Milz
Siehe auch:
- Splenomegalie
- Angiosarkom der Milz
- Lymphom der Milz
- Milzmetastasen
- Lymphangiom Milz
- Littoralzellangiom der Milz
- fokale Milzläsionen und Anomalien
- Milzhamartom
- inflammatorischer Pseudotumor der Milz
- Hämangioendotheliom Milz
- Differentialdiagnose eingeblutete Raumforderung Milz
- sklerosierende angiomatöse noduläre Transformation der Milz
- maligne Milztumoren
- fokale lymphatische Malformation der Milz
- Gefäßmalformation Milz
und weiter:

 Assoziationen und Differentialdiagnosen zu Raumforderungen der Milz:
Assoziationen und Differentialdiagnosen zu Raumforderungen der Milz:sklerosierende
angiomatöse noduläre Transformation der Milz