Chronische Pankreatitis
















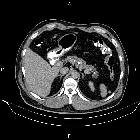














Chronic pancreatitis represents the end result of a continuous, prolonged, inflammatory and fibrosing process that affects the pancreas. This results in irreversible morphologic changes and permanent endocrine and exocrine pancreatic dysfunction.
Epidemiology
The most common cause of chronic pancreatitis in adults is excessive alcohol consumption in developed countries and malnutrition in developing countries .
Risk factors
The major risk factors for the development of chronic pancreatitis may be categorized according to the TIGAR-O system :
- T: toxic-metabolic (e.g. alcohol)
- I: idiopathic
- recent guidelines recommend that cystic fibrosis needs to be ruled out in these patients before calling it idiopathic
- G: genetic
- more commonly seen in the pediatric population
- A: autoimmune
- R: recurrent
- O: obstructive (e.g. choledocholithiasis, pancreatic head tumor)
Clinical presentation
Exacerbations (episodes of acute pancreatitis) may present with epigastric pain. These may recur over a number of years.
Symptoms may be attributable to the failure of:
- biliary outflow: jaundice
- exocrine function: malabsorption
- endocrine function: type 3c diabetes mellitus
Pathology
Acute pancreatitis and chronic pancreatitis are assumed to be different disease processes, and most cases of acute pancreatitis do not result in chronic disease.
Radiographic features
Please refer to the article on mass-forming chronic pancreatitis, for further details in this atypical presentation.
Ultrasound
The pancreas might appear atrophic, calcified or fibrotic (advanced stages). Findings that may be present on ultrasound include:
- hyperechogenicity (often diffuse) often indicates fibrotic changes
- pseudocysts
- pseudoaneurysms
- presence of ascites
Ultrasound may also assist to differentiate between the autoimmune type vs. acquired:
- the pancreas is enlarged (either focally or diffusely) in the autoimmune type
- calcifications are visible in acquired types
CT
CT features of chronic pancreatitis include:
- dilatation of the main pancreatic duct
- pancreatic calcification
- changes in pancreatic size (i.e. atrophy), shape, and contour
- pancreatic pseudocysts
MRI
May be undertaken both as morphological and functional imaging :
Morphological
Features of chronic pancreatitis can be divided into early and late findings:
-
early findings
- low-signal-intensity pancreas on T1-weighted fat-suppressed images
- decreased and delayed enhancement after IV contrast administration
- dilated side branches
- late findings
- parenchymal atrophy or enlargement
- pseudocyst formation
- dilatation and beading of the pancreatic duct often with intraductal calcifications, could give a 'chain of lakes' appearance.
Functional
Exocrine function may be assessed by secretin-enhanced magnetic resonance cholangiopancreatography, SMRCP (a.k.a. MRCP-S). This relatively new technique has shown promising results and may replace endoscopic measuring techniques in the near future . Imaging protocols to assess exocrine function may contain:
- measurement of secretory volume after intravenous secretin-stimulation by assessing T2-high signal changes in the duodenum
- post-enhanced dynamic assessment of ADC maps of pancreatic parenchyma, revealing delayed and reduced peak values
Radiology report
Standardized reporting terminology has been suggested for chronic pancreatitis. For more information see reference 11.
Treatment and prognosis
Pancreatic enzyme replacement therapy (PERT) has been recommended when there is clinical symptoms or laboratory signs of malabsorption . In those patients with refractory pain, in the presence of a dilated main pancreatic duct, endoscopic treatment should be considered, and surgery usually reserved as a second option.
After 20 years of chronic pancreatitis, there is a 6% cumulative risk of developing pancreatic adenocarcinoma.
Siehe auch:
- Pankreaspseudozyste
- Akute Pankreatitis
- Autoimmunpankreatitis
- Pankreas
- nekrotisierende Pankreatitis
- Pankreasverkalkungen
- haemorrhagic pancreatitis
- paraduodenale Pankreatitis
und weiter:
- Aneurysma spurium
- exsudative Pankreatitis
- Pankreatitis
- Chain of lakes sign
- Kometenschweif-Artefakte (Ultraschall)
- intraduktale papillär muzinöse Neoplasie
- posttraumatisches Aneurysma spurium
- Frey procedure
- chronische kalzifizierende Pankreatitis
- increased splenic density
- Gallengangsstrikturen
- pancreatic ductal carcinoma
- puestow procedure
- Farbdoppler-Kometenartefakt
- Kometenschweif-Zeichen
- Pankreatitis ohne Lipaseerhöhung
- chronisch obstruktierende Pankreatitis
- Konkrement im Pankreasgang
- splenic vein stenosis complicating chronic pancreatitis, recanalization with endoprosthesis prior to pancreatic surgery
- chronic pancreatitis and pseudocysts
- acute on chronic pancreatitis
- Milzvenenstenose

 Assoziationen und Differentialdiagnosen zu Chronische Pankreatitis:
Assoziationen und Differentialdiagnosen zu Chronische Pankreatitis:





