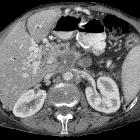
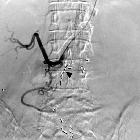
Akute Pankreatitis























Acute pancreatitis (plural: pancreatitides) is an acute inflammation of the pancreas and is a potentially life-threatening condition.
The diagnosis of acute pancreatitis is made by fulfilling two of the following three criteria :
- acute onset of persistent, severe epigastric pain (i.e. pain consistent with acute pancreatitis)
- lipase/amylase elevation >3 times the upper limit of normal
- characteristic imaging features on contrast-enhanced CT, MRI, or ultrasound
Imaging is only required to establish the diagnosis if the first two criteria are not met. Imaging is crucial for the detection of complications and to help guide treatment.
Terminology
There are two subtypes of acute pancreatitis as described by the Revised Atlanta Classification :
- interstitial edematous pancreatitis
- the vast majority (90-95%)
- most often referred to simply as "acute pancreatitis" or "uncomplicated pancreatitis"
- necrotizing pancreatitis
- necrosis develops within the pancreas and/or peripancreatic tissue
Epidemiology
The demographics of patients affected by acute pancreatitis reflects the underlying cause, of which there are many, including:
- gallstone passage/impaction: most common cause of acute pancreatitis (up to 15% develop pancreatitis)
- idiopathic: 20% (range 10%-30%) of cases of acute pancreatitis
- evidence suggests that most cases are associated with congenital duct abnormalities
- alcohol abuse: most common cause of chronic pancreatitis
- non-linear dose-response relationship
- 1.2x risk with ~40 g/day alcohol consumption
- 4x risk with ~100 g/day alcohol consumption
- non-linear dose-response relationship
- metabolic disorders
- hypertriglyceridemia-induced pancreatitis
- 1-4% of cases
- most common cause in pregnancy
- hypercalcemia
- hypertriglyceridemia-induced pancreatitis
- autoimmune pancreatitis
- penetrating peptic ulcer
- trauma: most common cause in children
- blunt abdominal trauma
- surgery
- endoscopic retrograde cholangiopancreatography (ERCP)
- malignancy
- hereditary pancreatitis (autosomal dominant) SPINK1 gene mutation
- malnutrition
- infection
- viral: mumps, Coxsackievirus, hepatitis, infectious mononucleosis, HIV/AIDS
- parasitic: ascariasis , clonorchiasis
- structural: not a cause, but associated with increased incidence
- toxins
- scorpion sting: in particular, the Trinidad thick-tailed scorpion, Tityus trinitatis
- spider bite (several species)
- snake bite (adder, cobra)
- drugs: steroids, tetracycline, frusemide, azathioprine, thiazides, L-asparaginase and many others
- interestingly, NSAIDs, while used for symptomatic treatment of pancreatitis, have been implicated as a possible cause, e.g. diclofenac is used in preventing post-ERCP pancreatitis, but is nonetheless considered the major NSAID responsible for inducing acute pancreatitis in the general population
- others
See: causes of pancreatitis (mnemonic)
Clinical presentation
Classical clinical features include :
- acute onset of severe central epigastric pain (over 30-60 min)
- poorly localized tenderness and pain
- exacerbated by supine positioning
- radiates through to the back in 50% of patients
Elevation of serum amylase and lipase are 90-95% specific for the diagnosis .
A normal amylase level (normoamylasaemia) in acute pancreatitis is well-recognized, especially when it occurs on a background of chronic pancreatitis. A normal lipase level has also been reported (<10 case reports) but is extremely rare .
(Rare) signs of hemorrhage on the physical exam include:
- Cullen sign: periumbilical bruising
- Grey-Turner sign: flank bruising
Pathology
There continues to be debate over the precipitating factor leading to acute pancreatitis, with duct occlusion being an important factor, but neither necessary nor sufficient.
Mechanism notwithstanding, activation of pancreatic enzymes within the pancreas rather than the bowel lead to inflammation of the pancreatic tissue, disruption of small pancreatic ducts and in leakage of pancreatic secretions. Because the pancreas lacks a capsule, the pancreatic juices have ready access to surrounding tissues. Pancreatic enzymes digest fascial layers, spreading the inflammatory process to multiple anatomic compartments.
Complications
- pancreatic fluid collections are defined by presence or absence of necrosis (as described by the Revised Atlanta Classification):
- necrosis absent (i.e. interstitial edematous pancreatitis)
- acute peripancreatic fluid collections (APFCs) (in the first 4 weeks)
- pseudocysts: encapsulated fluid collections after 4 weeks
- necrosis present (i.e. necrotizing pancreatitis)
- acute necrotic collections (ANCs): develop in first 4 weeks
- walled-off necrosis (WON): encapsulated collections after 4 weeks
- necrosis absent (i.e. interstitial edematous pancreatitis)
- liquefactive necrosis of pancreatic parenchyma (e.g. necrotizing pancreatitis)
- increased morbidity and mortality
- may become secondarily infected (emphysematous pancreatitis)
- vascular complications
- hemorrhage: resulting from erosion of blood vessels and tissue necrosis
- pseudoaneurysm: autodigestion of arterial walls by pancreatic enzymes results in pulsatile mass that is lined by fibrous tissue and maintains communication with parent artery
- splenic vein thrombosis
- portal vein thrombosis
- fistula formation with pancreatic ascites: leakage of pancreatic secretions into the peritoneal cavity
- abdominal compartment syndrome
Radiographic features
The role of imaging is manifold:
- to clarify the diagnosis when the clinical picture is confusing
- to assess severity (Balthazar score) and thus to determine prognosis
- to detect complications
- to determine possible causes
Imaging studies of acute pancreatitis may be normal in mild cases. Contrast-enhanced CT provides the most comprehensive initial assessment, typically with a dual-phase (arterial and portal venous) protocol. However, US is useful for follow-up of specific abnormalities, such as fluid collections and pseudocysts.
Plain radiograph
Radiographs are insensitive for evidence of acute pancreatitis: many patients have normal exams. Moreover, none of the signs are specific enough to establish the diagnosis of pancreatitis.
Abdominal radiographs may demonstrate:
- localized ileus of small intestine (sentinel loop)
- spasm of the descending colon (colon cut-off sign)
Chest radiographs may demonstrate:
- pleural effusion, usually left-sided
- hemidiaphragm elevation
- basal atelectasis
- pulmonary edema suggestive of acute respiratory distress syndrome
Ultrasound
The main role of ultrasound is:
- to identify gallstones as a possible cause
- diagnosis of vascular complications, e.g. thrombosis
- identify areas of necrosis which appear as hypoechoic regions
- assessment of clinically similar etiologies of an acute abdomen
In the event of a serendipitously patent acoustic window, typical ultrasonographic features congruent with acute pancreatitis include:
- increased pancreatic volume with a marked decrease in echogenicity
- volume increase quantified as a pancreatic body exceeding 2.4 cm in diameter, with marked anterior bowing and surface irregularity
- decreased echogenicity secondary to fluid exudation, which may result in a marked heterogeneity of the parenchyma
- displacement of the adjacent transverse colon and/or stomach secondary to pancreatic volume expansion
CT
Abnormalities that may be seen in the pancreas include:
- typical findings
- focal or diffuse parenchymal enlargement
- changes in density because of edema
- indistinct pancreatic margins owing to inflammation
- surrounding retroperitoneal fat stranding
- liquefactive necrosis of pancreatic parenchyma
- lack of parenchymal enhancement (should ideally be 1 week after symptom onset to differentiate from pancreatic hypoenhancement secondary only to edema)
- often multifocal
- infected necrosis
- difficult to distinguish from aseptic liquefactive necrosis
- the presence of gas is helpful (emphysematous pancreatitis)
- FNA helpful
- abscess formation
- circumscribed fluid collection
- little or no necrotic tissues (thus distinguishing it from infected necrosis)
- hemorrhage
- high-attenuation fluid in the retroperitoneum or peripancreatic tissues
- calcification
- evidence of background chronic pancreatitis
Dual-energy CT
Dual-energy CT may be able to help better differentiate necrotic debris, hematoma and areas of viable tissue in cases of necrotizing pancreatitis. In hemorrhagic pancreatitis, virtual non-enhanced images can depict hematoma and differentiate it from parenchymal enhancement on contrast-enhanced images. It also improves detection of non-calcified gallstones and isoattenuating cholesterol stones which may be the causative factor in the patient's pancreatitis .
Dual-energy CT dual-phase protocols with a virtual non-enhanced reformat can also offer lower radiation doses than conventional triple-phase CT imaging of the pancreas .
MRI
Contrast-enhanced MR is equivalent to CT in the assessment of pancreatitis.
Treatment and prognosis
Treatment is largely supportive, often requiring ICU care in severe cases for respiratory and cardiovascular support and careful management of glucose, calcium, and fluid balance.
Recommendations include :
- aggressive fluid resuscitation in first 24 hours
- no need for prophylactic antibiotics
- enteral feeding strongly preferred over parenteral feeding, especially in severe acute pancreatitis
- no need for ERCP in acute gallstone pancreatitis unless evidence of ascending cholangitis
- image-directed catheter placement is an alternative to surgical drainage of pancreatic fluid collections
- cholecystectomy before discharge in patients with acute pancreatitis and gallstones found on imaging
Prognosis for acute pancreatitis varies according to severity. Overall mortality is 5-10% per attack . Various scoring systems exist that attempt to stratify severity (e.g. Ranson's criteria and APACHE II).
The 2012 revised Atlanta classification attempts to establish uniformity in reporting for both clinical practice and research .
Differential diagnosis
General imaging differential considerations include:
- pancreatic ductal adenocarcinoma
- autoimmune pancreatitis
- peptic ulcer disease with posterior perforation
- pancreatic lymphoma (diffuse pattern)

 Assoziationen und Differentialdiagnosen zu Akute Pankreatitis:
Assoziationen und Differentialdiagnosen zu Akute Pankreatitis: