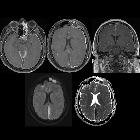
empyema
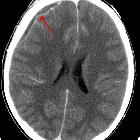
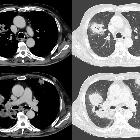






Empyemas are purulent inflammatory collections within a body cavity. Contrast this with abscesses, which arise within parenchymal tissue, rather than occupying a pre-existing anatomical space.
Terminology
Colloquially, the standalone term empyema is used to refer to thoracic empyemas but there are various different types of empyema which are described by the organ affected:
- gallbladder empyema
- subdural empyema
- thoracic empyema
- joint empyema (of any synovial joint)
- empyema cystitis (urinary bladder)
Pathology
Empyemas are predominantly caused by bacterial infection of fluid within a pre-existing anatomical space. Once significant bacterial translocation has occurred there is significant deposition of fibrin and a reactive inflammatory response, which results in the accumulation of pyogenic and fibrous material within the cavity.
The pathogenesis of an empyema usually requires a small stagnant fluid collection. In the case of the gallbladder, this requires a degree of biliary tract obstruction.
Treatment and prognosis
Like abscesses, as the vascular supply to an empyema is poor, antimicrobial treatment on its own is usually insufficient to treat the underlying infection and drainage of the collection is usually required. This is often done percutaneously with ultrasound guidance, although open surgical drainage may be necessary in complex cases.
In cases of empyema involving synovial joints, surgical washout can often be the preferred treatment method, since the preservation of joint surfaces from infection-related damage or the post-infectious inflammatory process is important to preserve function.
Differential diagnosis
- abscess
- loculated pleural effusions
- sterile fluid collection
See also
Siehe auch:
und weiter:
- axiale Hiatushernie
- subdurales Hygrom
- Hiatushernie
- Phrenikusparese
- Lungenabszess
- Clagett thoracotomy
- einzelne Pleuraraumforderung
- Pleuraplaques bei Asbestose
- tuberculous empyema
- Serothorax
- Thorax Onlinekurs
- differential of a large unilateral pleural effusion
- Pleuraempyem vs. Lungenabszess
- Schulterempyem
- Pleura-Split-Zeichen (Empyem)

 Assoziationen und Differentialdiagnosen zu Empyem:
Assoziationen und Differentialdiagnosen zu Empyem: