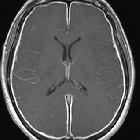
subdural empyema
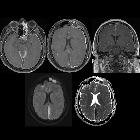
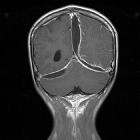















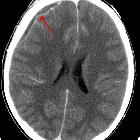

Subdural empyema is a type of intracranial infection characterized by a suppurative collection between the dura mater and arachnoid mater. It is commonly seen as a complication of sinusitis, otitis, mastoiditis, or surgical intervention.
On imaging, it tends to present as a subdural collection, crescentic in shape, with marked meningeal enhancement and, on MRI, typically demonstrates restricted diffusion.
Epidemiology
Subdural empyemas account for approximately 20-33% of all intracranial infections.
Clinical presentation
Clinical presentation depends to some degree on the etiology. When empyemas result from sinusitis or mastoiditis they are often associated with seizures, focal neurological deficits and rapid deterioration of consciousness, progressing from obtundation to coma . Empyemas that occur secondary to prior trauma or surgery are usually more clinically indolent.
Pathology
In the most common scenario, patients develop subdural empyemas as a result of frontal sinusitis. There are two putative mechanisms of spread :
Direct spread, resulting from erosion of the posterior wall of the frontal sinus (the corollary of Pott puffy tumor) is relatively uncommon. Thrombophlebitis of communicating veins is thought to be the most common cause of spread .
Etiology
- frontal sinusitis: vast majority
- mastoiditis/otitis media
- surgical intervention
- meningitis
- trauma
- seeding of existing subdural hematoma
Radiographic features
CT is usually the first investigation performed and often is the only one required, as patients usually expediently proceed to the surgical theater for evacuation.
CT
Subdural empyemas typically resemble subdural hematomas in their shape and the relationship to sutures and dural reflections. They are typically crescentic in shape (compared to epidural empyemas which are typically lentiform), although collection pockets may appear biconvex (see case 1). A surrounding membrane that enhances intensely and uniformly following contrast administration is typical.
MRI
Appearance on MRI is similar to that on CT, although contrast enhancement is more readily detected. Furthermore, the content of the collection will typically demonstrate restricted diffusion (see case 1).
MRI is also more sensitive to the complications of subdural empyemas, e.g. cerebritis, cerebral abscess, and venous thrombosis.
Treatment and prognosis
Mortality associated with subdural empyemas now approaches 10%, compared with approximately 15-40% in the pre-CT era .
Successful treatment is predicated on prompt diagnosis, followed by surgical evacuation of the collection and administration of appropriate antibiotics.
Complications
Complications are relatively common and may be the cause of presentation. They include:
- cortical vein thrombosis with or without venous infarction
- cerebritis or cerebral abscess formation
Siehe auch:
- Arachnoidalzyste
- Hirnabszess
- subdurales Hämatom
- Empyem
- Meningitis
- Mastoiditis
- Hygrom
- intrakranielle Infektionen
- chronisches Subduralhämatom
- venous infarction
- epidural empyemas
und weiter:

 Assoziationen und Differentialdiagnosen zu subdurales Empyem:
Assoziationen und Differentialdiagnosen zu subdurales Empyem: